Pericoronitis Treatment
Inflammation in the area of erupting teeth is one of the most common reasons for visiting an oral surgeon. Timely treatment of pericoronitis helps prevent the spread of infection to adjacent tissues.

specialists

equipment

treatment

Causes and risk factors
The main cause of the disease is a disruption to the natural process of tooth emergence. There are several factors that contribute to this process.
Difficult Wisdom Tooth Eruption
Third molars often lack space in the jaw arch. Because of this, difficult tooth eruption can be delayed for months or years. While the crown remains submerged, the gums remain vulnerable to infection. If the tooth is misaligned (at an angle), it can traumatize soft tissue for years, causing chronic inflammation.
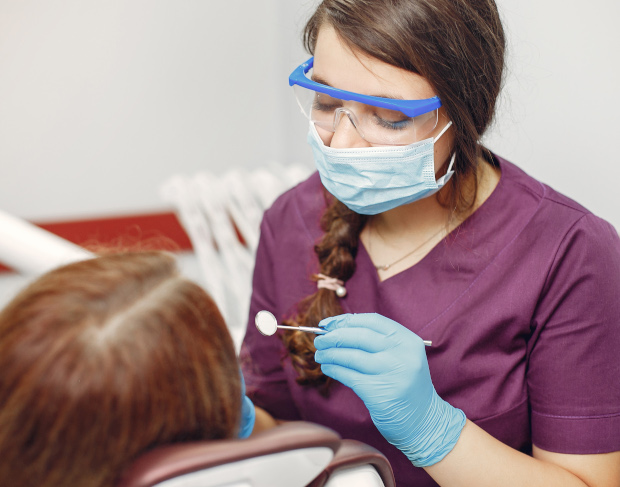
Accumulation of plaque and food debris under the hood
Microscopic food particles and soft plaque accumulate under the gingival fold. Since they cannot be cleaned out, decay begins. This leads to inflammation of the wisdom tooth hood. Pathogenic microflora actively proliferates in the gingival pocket, triggering an immune response in the form of swelling and pain.
Gum trauma and other triggering factors
Constant mechanical stress also plays a role. During chewing, the opposing upper tooth can bite down on the swollen gingival hood, increasing trauma and accelerating the development of infection. Additional risk factors include decreased overall immunity, acute respiratory infections, and poor oral hygiene.
The clinical picture of the disease depends on the stage of the process. There's no need to endure pain: it's much easier to solve the problem at the initial stage.
At the first stage, discomfort appears. After a day or two, symptoms of pericoronitis appear: slight redness of the gum margin and aching pain that intensifies when chewing hard foods. Swelling of the gums may also occur; this doesn't interfere with opening the mouth yet, but it is already causing discomfort.
If treatment is not provided promptly, purulent pericoronitis develops. The pain becomes throbbing, often radiating to the ear or temple. A pronounced foul odor from the mouth develops, associated with exudate secreted from under the gums. Swelling spreads to the cheek and submandibular lymph nodes. At this stage, pain is often felt when opening the mouth, as the inflammation affects the masticatory muscles.
Self-medication in such cases is life-threatening. The purulent lesion is located near the nose and eyes, so you should see a doctor if:
- Pain near the wisdom tooth increases
- Swelling of the gums or cheek
- Pain when opening the mouth
- Foul odor or taste in the mouth
- Pus
- High fever
Do not warm the cheek. Self-administration of antibiotics is also not recommended: this problem can be solved with less conservative measures.
Diagnostics
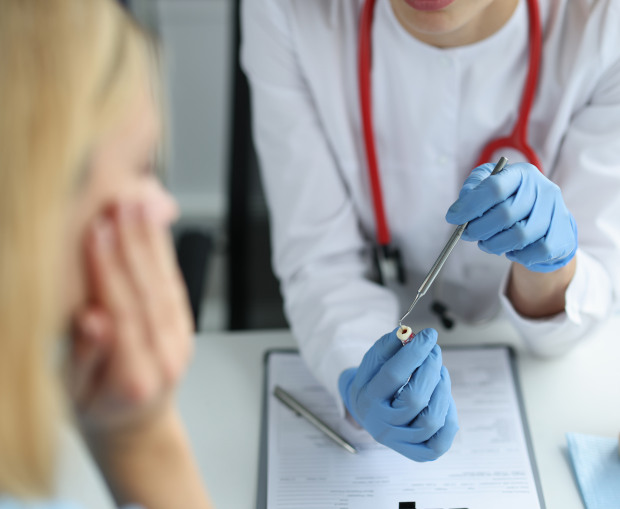
An accurate diagnosis is made by an oral surgeon based on the clinical picture and instrumental examination data. Diagnostics are necessary to distinguish the disease from problems with adjacent teeth.
Oral examination and collection of complaints
The doctor assesses the degree of redness, the presence of purulent discharge, and the condition of adjacent teeth. Lymph node tenderness is also checked. During the examination, the severity of the gum inflammation around the wisdom tooth is determined and whether there are signs of involvement of surrounding tissues.
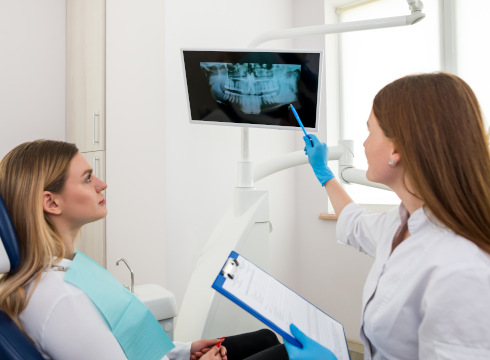
X-ray or CT scan as indicated
Visual examination is not enough to determine the treatment strategy. The doctor needs to understand the tooth's position in the bone. For this, an X-ray of the wisdom tooth (a targeted or panoramic image) or a computed tomography (CT) scan is performed. The image shows whether there is enough room for the tooth to erupt or whether it is pressing against the adjacent tooth, causing recurrence.
Treatment methods for pericoronitis
The treatment strategy depends on the tooth's location and the severity of the inflammation. The dentist may choose a conservative approach or surgical intervention.
Rinsing and Antiseptic Treatment
In the earliest stages, antiseptic treatment is helpful. During the procedure, the doctor removes food debris from under the hood and applies a solution. This is not a complete treatment, but a temporary measure.
Hood Excision
If the tooth is correctly positioned and has sufficient space in the jaw, a hood excision is performed. The surgeon removes the overhanging mucous membrane that covers the crown. After the wisdom tooth hood is removed, the pocket for bacteria disappears, and the tooth can continue to erupt unhindered.
Wisdom tooth removal according to indications
In cases where there is no room in the jaw or the tooth lies horizontally, pericoronitis of the wisdom tooth will recur. The only way to resolve the problem is wisdom tooth removal.
| Method | When used | Treatment goal | Recovery features |
|---|---|---|---|
| Rinse and antiseptic treatment | At initial inflammation | Reduce inflammation and cleanse the hood area | Monitor the condition; relapse is possible without tissue removal |
| Excision of the hood | If the hood is constantly injured and retains food | Eliminate the source of recurrence Inflammation | Local intervention, soft tissue healing in 3-5 days |
| Wisdom tooth removal | In case of malpositioned teeth and recurrence | Remove the cause of inflammation | Recovery time longer than with local treatment eliminates recurrence |
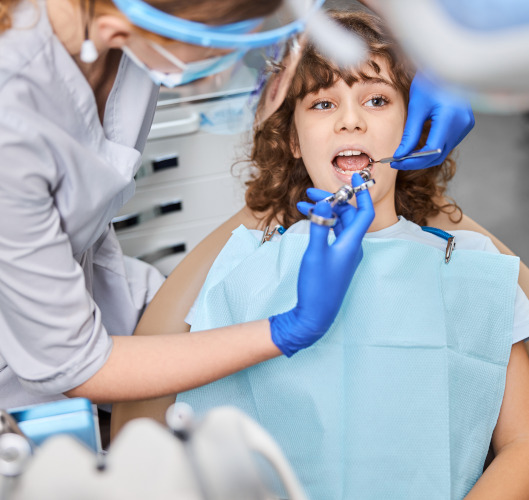
How the treatment is performed
The procedure usually takes 15 to 40 minutes. Modern technologies make the process painless.
Preparation and pain relief
Any treatment for gum inflammation above a wisdom tooth begins with anesthesia. Medications that completely block sensitivity are used. Before the injection, the gum may be treated with an anesthetic gel.
Main stages of the procedure
Hood excision is a surgical procedure performed by a surgeon. If the tooth can be saved, the doctor simply removes the hood and pus. If the tooth cannot be saved, it is extracted. Next, the wound is cleaned and sutured (if necessary).
What to do after treatment
Immediately after your appointment with the doctor, it is important to rest. Do not eat or drink until the anesthesia wears off. During the first 24 hours, you can apply a cold compress to your cheek for 5-10 minutes to reduce postoperative swelling.
Recovery and prevention
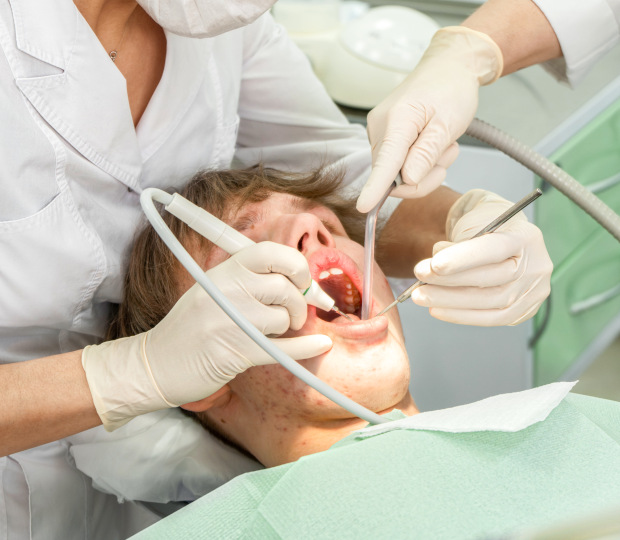
The recovery period after pericoronitis treatment lasts from several days to a week.
What to do and what not to do after the procedure
For the first 2-3 days, avoid heating the inflamed area or visiting baths or saunas. A soft diet is recommended. Avoid vigorous mouth rinsing; only gentle "mouth baths" with an antiseptic are allowed.
How to reduce the risk of recurrence
Good hygiene is essential. Brush your teeth. If your doctor has recommended wisdom tooth extraction after the acute inflammation has subsided, do not delay this procedure.
Possible complications without treatment
If you ignore the symptoms of pericoronitis, the infection can spread to adjacent tissues. The most dangerous consequences include abscesses and cellulitis. Complications of pericoronitis may also include inflammation of the jaw bone (osteomyelitis) or lymph node damage.
Pericoronitis is a problem that can't be treated at home. It's best treated at the dentist's office. Don't delay going to the dentist: the longer you wait, the more expensive the treatment will be.
Frequently Asked Questions
Is it possible to treat gum inflammation around a wisdom tooth on your own?
No, rinsing and soaking in medicated mouthwash will simply relieve the pain. They won't eliminate the underlying cause. The infected gum pocket needs to be cleaned. Without a doctor's attention, the condition will become chronic or purulent.
Is hood excision painful?
The procedure is performed under local anesthesia, so there is no pain during the procedure. Minor discomfort after the freezing process wears off can be easily relieved with regular painkillers.

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Price






















































































What is pericoronitis?
Pericoronitis is an inflammation of the gums around a partially erupted tooth. In the vast majority of cases, this condition affects the lower third molars. When a tooth partially erupts, a hood forms over the wisdom tooth's chewing surface.
This hood doesn't adhere tightly to the enamel, and this open space is an ideal breeding ground for bacteria. This area is difficult to reach, so pus quickly develops.