Herpetic Stomatitis: Symptoms, Causes, and Treatment
Herpetic stomatitis begins suddenly. A burning sensation, weakness, and pain develop. Small lesions, which eventually develop into erosions, appear on the mucous membrane. Eating and drinking become difficult. Even talking causes discomfort. Brushing teeth also causes pain.
The first signs of the disease can be confused with other illnesses, so diagnosis and treatment of herpetic stomatitis are only performed in person by a specialist.
Diagnosis and treatment of herpetic stomatitis are only performed in person.

specialists

equipment

treatment
Herpetic stomatitis is an inflammation of the oral mucosa that develops as a result of an infection caused by the herpes simplex virus. After the initial episode, the virus does not disappear from the body: it persists in nerve cells and, under favorable conditions, can cause a relapse.
For this reason, the diagnosing physician evaluates not only the erosions but also the patient's well-being and the condition of their gums, lips, and the entire oral mucosa.
How does herpetic stomatitis differ from other types of stomatitis?
Similarities with other illnesses are noticeable within the first few days. Some patients mistake the process for a reaction to food, others for an injury to the mucosa, and still others for ordinary wounds.
Aphthous stomatitis consists of isolated, painful ulcers without blisters. Candidiasis is characterized by white plaques that, when removed, reveal wound surfaces. The herpetic form presents as ulcers with blisters.
| Form | Cause | Appearance | Localization | Infectivity |
|---|---|---|---|---|
| Herpetic | Herpes simplex virus | Blisters → Erosions | Oral cavity, lips, gums | High during the acute period |
| Aphthous | Immune and local triggers | Single aphthae | Inner lips and cheeks | Usually none |
| Candidal | Candida fungi | White patches, red areas | Tongue, cheeks, palate | Depends on the cause |
The table is for quick reference, but the final conclusion is based on the examination, complaints, and the progression of the process.
Acute and recurrent variants
The acute stage of the disease is severe. The lesions are large, the body temperature is high, and the pain is quite severe.
In a relapse, the disease is localized; the ulcers do not interfere with eating, drinking, or maintaining hygiene, but they still cause discomfort.
Symptoms of herpetic stomatitis
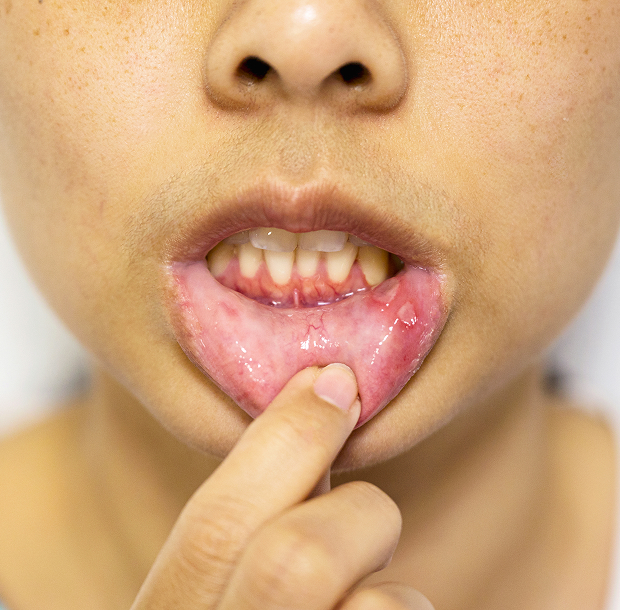
The clinical picture develops in stages. General complaints begin, then lesions appear on the mucous membrane, and later, painful erosions and ulcers form in the mouth.
First signs of the disease
The onset often resembles a viral infection. Burning sensations, weakness, refusal to eat solid foods, and sometimes headache and fever occur. Some patients experience enlarged submandibular or cervical lymph nodes.
What do blisters, erosions, and ulcers look like?
Initially, small blisters appear on the mucous membrane in the mouth. They quickly burst, leaving painful erosions with a red border. Oral herpes causes pain that intensifies with swallowing.
Characteristics of symptoms in children and adults
The initial episode in children is often more severe due to pain and refusal to drink water. Therefore, herpetic stomatitis in children is dangerous due to the risk of dehydration.
In adults, herpetic stomatitis usually occurs locally, without extensive mucosal damage. But even in this form, it can cause a severe burning sensation, pain during eating, and a noticeable deterioration in well-being. If relapses occur in a child, it is important for the doctor to assess the frequency of flare-ups and understand what triggers them.
Causes and Routes of Transmission
The disease is caused by the characteristics of the herpes simplex virus and its transmission routes—through saliva or the contents of lesions. Once in the body, the virus persists for a long time and can eventually reactivate.
Pathogen: Herpes Simplex Virus
Herpetic stomatitis is most often caused by the herpes simplex virus type 1 (HSV-1). It infects the mucosal epithelium, causing painful rashes. After the initial episode, the infection does not clear completely: the virus remains in the body in an inactive form. Its reactivation is possible with colds, stress, mucosal trauma, overheating, hypothermia, and a weakened immune system.
How does infection occur?
The virus is most often transmitted through everyday life and close contact—through saliva, kissing, sharing utensils, and hygiene products. The risk is associated not only with severe symptoms of the disease. Transmission is also possible when there are no symptoms or they are mild. Therefore, doctors usually explain to patients how contagious herpetic stomatitis is.
Risk factors and causes of exacerbation.
The disease recurs after an acute respiratory viral infection, as well as due to regular sleep deprivation, severe stress, or local trauma. Gum inflammation and chronic irritation negatively affect the condition of the oral mucosa.
Prevention
The risk cannot be completely eliminated because the virus persists in the body. However, the frequency of recurrent episodes can be reduced and the course of the illness can be milder.
Oral hygiene
Good oral hygiene helps maintain a calmer mouth, control plaque, and reduce unnecessary irritation. During an exacerbation, use a soft brush and gentle brushing.
How to reduce the risk of recurrent episodes
Sleep, fluid intake, stress management, eliminating traumatic factors in the mouth, and avoiding the use of common hygiene products during the acute phase are helpful. If relapses are frequent, the doctor may reconsider the monitoring strategy.
Strengthening local mucosal defenses
Good nutrition, gentle oral hygiene, and correcting underlying disorders are important for local defense. During recurrent outbreaks, it is helpful to assess deficiencies, coexisting illnesses, and immune status.

FAQ
The short answers below are intended to provide guidance, but are not intended to replace an in-person consultation.
Is herpetic stomatitis contagious?
How long does herpetic stomatitis last?
How does it differ from aphthous sores?
Treating a disease at home: is it possible or not?
Warning: If you experience severe pain, high fever, signs of dehydration, or a worsening general condition, seek medical attention as soon as possible.
Caution! This material is for informational purposes only. Do not self-medicate. At the first sign of illness, consult a doctor.

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Price







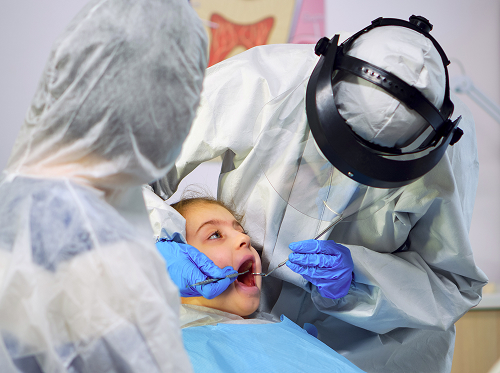
















































































Diagnostics
The doctor diagnoses the patient based on the overall clinical picture. Naturally, the specialist listens to the patient's complaints, thereby monitoring the dynamics of symptoms. During a visual examination, the specialist evaluates the type of ulcers and their location. The doctor also determines whether there was pain, whether there was a fever, and whether similar episodes have occurred previously.
When is differential diagnosis necessary?
Uncertainties often arise with an atypical course of the disease, a protracted process, or isolated erosions, if the usual vesicular rash is absent. In such situations, the doctor conducts differential diagnosis to distinguish herpetic stomatitis from aphthous stomatitis, candidiasis, traumatic mucosal lesions, and enterovirus infection.
When may additional testing be needed?
PCR diagnostics are performed only in cases of severe disease, immunodeficiency, or a questionable clinical picture.