Cheilitis Treatment
Treatment begins with identifying the cause of the condition. Lip inflammation causes severe discomfort, interfering with speech, eating, and smiling. The problem often recurrs with improper treatment.
Our clinic offers a comprehensive approach to treating inflammation: identifying the cause, selecting an individualized treatment plan, and recommending care and relapse prevention. Cheilitis of the lips requires the careful attention of a medical professional.

specialists

equipment

treatment
Symptoms and Signs of Cheilitis
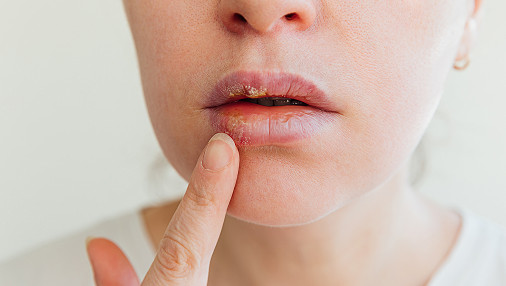
The clinical presentation depends on the form of the disease. Symptoms of cheilitis include severe discomfort. Patients complain of dry lips and tightness of the skin. Redness and swelling of the tissues are also visible.
Severe peeling of the lips often occurs. Painful micro-tears appear on the surface. Cracks in the lips may bleed when talking or eating. Crusts sometimes form on the lips, and itching, burning, and general soreness occur. Cheilitis symptoms significantly impair quality of life.
Causes of Cheilitis
The factors that trigger the disease are extremely varied. The causes of cheilitis are divided into internal and external. External triggers include harsh weather conditions: frost, wind, and strong sun.
Contact dermatitis—an allergic reaction to irritants—plays a huge role.
Triggers include:
- Decorative cosmetics
- Aggressive toothpaste
- Food
Internal factors include decreased immunity, B vitamin deficiency, and chronic endocrine disorders. Infection (bacteria, fungi) causes specific tissue damage. The habit of licking or biting the skin aggravates the situation.

Types of cheilitis
Angular cheilitis
Colloquially known as cracks in the corners of the mouth, angular cheilitis affects the commissures. Microcracks appear, which become coated with plaque. The main culprits are streptococcal infection, fungus, and weakened immune defenses.
Allergic and contact cheilitis
The condition occurs due to contact with an irritant. Allergic cheilitis develops as an immune response to allergens. Triggers include lipstick, metal from wind instruments, and food. Severe swelling, redness, and small blisters occur.
Atopic cheilitis
This condition is a symptom of neurodermatitis or atopic dermatitis. Atopic cheilitis is characterized by lesions of the vermilion border of the lips, as well as the adjacent skin of the face. Severe itching, dry lips, and tissue thickening are observed.
Exfoliative cheilitis
This condition affects only the mucous membrane and the vermilion border. Exfoliative cheilitis is accompanied by the formation of abundant scales. Patients constantly peel off the scales, exposing the inflamed surface. The condition is closely associated with psycho-emotional overstrain, stress, and thyroid dysfunction.
Actinic and meteorological cheilitis
Inflammation occurs due to climatic factors. Ultraviolet radiation, wind, and cold provoke roughening of the skin. The surface becomes covered with fine scales.
Candidal cheilitis
Caused by yeast-like fungi of the genus Candida, candidal cheilitis develops as a result of antibiotic use or a weakened immune system. A characteristic symptom is a whitish coating concealing bright red, inflamed tissue.
Types of Cheilitis and Their Characteristics
| Type of Cheilitis | Main Symptoms | Possible Causes | What the Doctor Asks During Diagnosis |
|---|---|---|---|
| Angular | Cracks in the corners of the mouth, pain when opening the mouth | Bacteria, fungi, iron deficiency | Dentures, diet |
| Allergic | Swelling, redness, small rash, itching | Cosmetics, Toothpaste, metals | Recent change of hygiene products, contact with allergens |
| Atopic | Itching, dryness, skin lesions around the mouth | Genetic predisposition, allergies | Presence of atopic dermatitis, bronchial asthma |
| Exfoliative | Dense scales, burning, constant peeling | Stress, endocrine disorders | Psycho-emotional state, habit of biting lips |
| Candida | White coating, redness, Itching | Fungal infection, decreased immunity | Taking antibiotics, presence of oral thrush |
Diagnosing Cheilitis
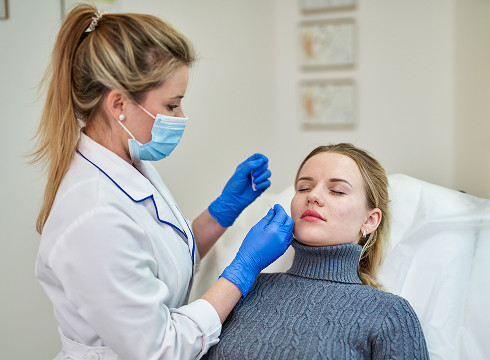
An accurate diagnosis is the key to successful treatment. The examination involves several stages.
Examination and History
The doctor carefully examines the affected area. The nature of the scaling and the presence of ulcers are assessed. The doctor determines the duration of the symptoms, the connection with external factors, and the presence of concomitant pathologies.
A specialist differentiates the disease:
- Herpes
- Contact dermatitis
- Systemic lupus erythematosus
- Candidiasis
When tests and additional examinations are needed
Instrumental diagnostics are used for complex clinical pictures. To detect fungi or bacteria, a scraping is taken from the surface. Blood tests can detect micronutrient deficiencies, allergy markers, and inflammatory processes.
General information
Frequently Asked Questions
What is cheilitis and how does it differ from regular dry lips?
Which doctor treats cheilitis?
Can cheilitis be treated at home?

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Price

























































































Which doctor treats cheilitis?
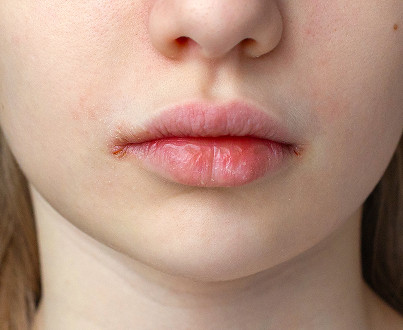
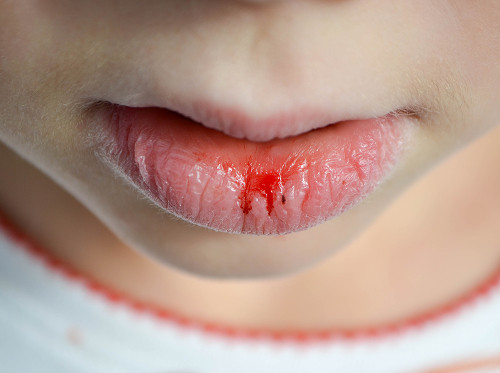
If you notice signs of inflammation, you should make an appointment with a specialist. But which doctor should you see? A dentist or dermatologist performs the initial diagnosis. The specialist assesses the condition of the tissues and collects the patient's complaints.
Sometimes, the help of specialized specialists is needed. If an allergy is suspected, the patient is referred to an allergist.