Treatment of ulcerative stomatitis in Moscow
Ulcerative stomatitis in Moscow often leads to emergency appointments when painful lesions appear in the mouth and eating, speaking, and brushing become difficult. Similar complaints can mask traumatic ulcers, aphthous ulcers, herpetic lesions, and gum disease. Therefore, treatment of ulcerative stomatitis begins with an examination and determination of the underlying cause.

specialists

equipment

treatment
Symptoms and signs of ulcerative stomatitis
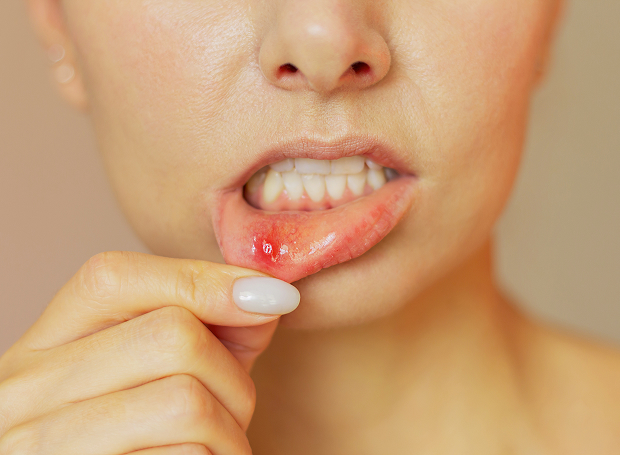
The first symptoms often become annoying within the first 24 hours. It can be difficult to eat hot, sour, and spicy foods, speak, and perform oral hygiene without pain.
What does ulcerative stomatitis look like?
Ulcerative stomatitis in the mouth can present in various ways. Sometimes it's a single ulcer with a red border left by biting the cheek. Other times, it's multiple lesions on the mucous membrane with plaque and severe inflammation around it. It's difficult to reliably distinguish the form of the disease from a single photograph.
Pain, plaque, bleeding, bad odor
For the patient, the most noticeable symptoms of ulcerative stomatitis are pain when eating, a burning sensation, plaque on the surface of the ulcer, bleeding gums, and bad breath. In more severe cases, weakness, lymph node swelling, and sometimes fever may occur.

When the condition requires urgent attention
An urgent appointment is needed when pain interferes with drinking, ulcers rapidly enlarge, a fever persists, swelling increases, or general condition worsens. It's also worth seeing a doctor quickly if lesions don't heal for more than two to three weeks or recur.
- Severe pain that makes eating and drinking difficult
- Severe swelling of the mucous membrane or gums
- Fever, weakness, swollen lymph nodes
- Rapid spread of lesions
- Ulcers don't heal or become deeper

Causes and risk factors
The causes of ulcerative stomatitis are always analyzed separately. The same defect can be associated with local trauma, infection, poor hygiene, or a general illness.
Infectious causes
In some cases, the inflammatory process is associated with bacterial flora against a background of soft plaque, tartar, and gum inflammation. This is how ulcerative necrotic stomatitis often develops. Viral infections are also possible, which, based on complaints, are similar to the ulcerative form, but require a different approach.
Mucosa trauma and hygiene problems
A common cause is trauma to the mucosa from a sharp tooth edge, an overhanging filling, hard food, or an ill-fitting toothbrush or appliance. If the trauma is accompanied by poor oral hygiene, plaque, and gum inflammation, healing is slower.
Decreased immunity and concomitant diseases
The risk is higher after:
- Severe stress
- Lack of sleep
- Smoking
- Deficiency conditions
- Chronic gastrointestinal diseases
- Diabetes
- Conditions with a reduced immune response
Recurring ulcers are sometimes associated with more than just the mucous membrane, so the doctor may recommend additional testing.
Diagnosis of ulcerative stomatitis
Diagnosis of ulcerative stomatitis is based on an in-person examination. The doctor evaluates not only the ulcers themselves on the oral mucosa, but also the condition of the gums, plaque, restorations, bite, and the entire oral mucosa.
Dentist examination and collection of complaints
During the initial appointment, the doctor asks when the pain began and whether there was a fever, injury, cold, chronic illness, smoking, or medication use. An oral examination is then performed. The location, depth, and appearance of the ulcer edges, the presence of plaque, and the condition of the gums are important for diagnosis.
How does ulcerative stomatitis differ from other forms?
For the patient, many lesions are similar, but the treatment approach is different. Ulcerative stomatitis differs from the catarrhal form by a deeper tissue defect. It differs from aphthous stomatitis by its relationship to the condition of the gums and the overall picture. It differs from herpetic lesions by the type of lesions. A traumatic ulcer is more often associated with a specific irritant in one area.
| Form | Main manifestations |
|---|---|
| Ulcerative stomatitis | Deep, painful lesions, plaque, severe inflammation |
| Aphthous stomatitis | Small, rounded aphthae, moderate pain, recurrence |
| Catarrhal stomatitis | Redness and swelling without deep ulcers |
| Traumatic ulcer | Localized defect near the source of injury |
| Herpetic lesion | Groups of elements, soreness, possible fever |
When additional testing may be needed
Not everyone needs additional testing. They are prescribed if ulcers frequently recur, take a long time to heal, the presentation is atypical, or there is a suspicion of a general disease. For persistent suspicious lesions, the scope of the examination is expanded.
Prevention is based on clear measures: meticulous hygiene, regular checkups, prompt treatment of cavities and gum disease, cessation of harmful habits, and correction of risk factors. If ulcers have occurred previously, it is useful to discuss recurrence triggers with your doctor.
FAQ
What is aphthous stomatitis?
Is it possible to treat canker sores at home?
How long does treatment for ulcerative stomatitis last?
When is an urgent consultation needed?
The information in this material is for reference only and does not replace an in-person consultation. If you experience pain, fever, increasing swelling, severe plaque, or any worsening of your condition, consult a doctor.

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Price
























































































What is ulcerative stomatitis?
An inflammatory lesion in which painful lesions of varying depth form on the mucous membrane is called ulcerative stomatitis. A doctor, when examining mouth ulcers, evaluates their depth, plaque, and bleeding. They also look for a connection with the condition of the gums. In everyday life, any ulcers on the oral mucosa are called stomatitis.
Ulcerative necrotic stomatitis is a separate condition. It is characterized by severe pain, gray-white plaque, bleeding, odor, and areas of necrosis in the interdental papillae and marginal gingiva. This condition requires immediate medical attention.