Oral lichen planus
Diseases of the oral mucosa often cause significant discomfort, as the oral cavity is involved in eating, speaking, and breathing. Among chronic pathologies, oral lichen planus occupies a special place – a condition that can go unnoticed for years or, conversely, cause severe pain.

specialists

equipment

treatment
Symptoms of oral lichen planus

Manifestations of the disease depend on its form, but there are classic signs that allow a doctor to suspect the diagnosis already at the first examination.
White reticular streaks and plaques on the mucous membrane
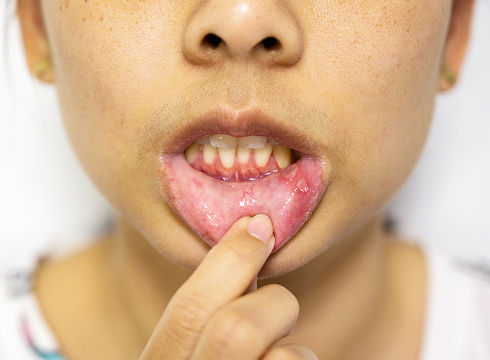
The main visual sign is small white or grayish-white papules. They intertwine, forming a pattern resembling lace, web, or mesh. These formations are either flat or slightly raised above the surface. In some cases, they can merge into dense white plaques resembling leukoplakia.
Burning, pain, discomfort when eating
In mild forms, the patient may not notice any changes at all, discovering the streaks accidentally in a mirror. However, as the disease progresses, a persistent burning sensation in the mouth develops, which intensifies with the consumption of acidic, spicy, salty, or hot foods. The mucous membrane becomes more sensitive, making every meal a torture.
Erosions, ulcers, redness, and swelling
In more severe cases, bright red areas—erosions—appear against the white mesh. These are areas where the protective epithelial layer has been destroyed. They can bleed at the slightest contact, such as when brushing your teeth. The surrounding tissue appears swollen and tense.
Causes and risk factors
Modern medicine views LP as a multifactorial disease. A single, precise cause has not yet been established, but in most cases, it is related to a weakened immune system.
Immune and chronic inflammatory mechanisms
The main theory behind its development is immunological. For unknown reasons, T lymphocytes (immune cells) begin to recognize cells in the basal layer of the epithelium as foreign and destroy them. This causes chronic inflammation of the mucosa, which is self-perpetuated by the body.
Mucosa trauma, dentures, sharp teeth edges
Constant trauma to the mucosa is the main cause of the disease's spread.
Most often, this occurs due to:
- Bad (or old) fillings with sharp edges
- Metal crowns (cause microcurrents - galvanism)
- Improperly fitted dentures
- Biting cheeks or lips
Drug, contact, and lichenoid reactions
Sometimes, oral rashes are not true lichen, but a so-called lichenoid reaction to components of toothpastes, mouthwashes, or denture materials. Also, some medications for the treatment of hypertension, diabetes, or arthritis can cause mucosal damage as a side effect.
Stress, comorbidities, bad habits
Psycho-emotional stress often precedes the first episode of the disease or a relapse. Furthermore, the causes of lichen planus in the mouth are often associated with gastrointestinal diseases, liver diseases, diabetes, and hormonal changes. Smoking and alcohol are other triggers that can lead to the disease.
Forms of oral lichen planus
The clinical presentation of lichen planus is extremely varied. For ease of diagnosis, doctors distinguish several main forms, which can transition from one to another.
| Form | What it looks like | Main complaints | Severity of discomfort |
|---|---|---|---|
| Typical reticular | Small white lines ("lace") on the cheeks and tongue | Usually asymptomatic | Minimal or absent |
| Erosive-ulcerative | Bright red wounds against a background of white stripes | Severe pain, burning, bleeding | Very high |
| Atrophic | Redness and thinning of the mucosa without ulcers | Soreness, dryness, sensitivity to heat | Moderate |
| Hyperkeratotic | Dense white plaques with clear edges | Sensation of roughness, "excess tissue" | Low, but requires monitoring |
Typical reticular form
This is the most favorable variant. The patient notices a white mesh that is painless. The mucosa retains its normal color, and there is no swelling. There is only one treatment: observation and elimination of irritants.
Erosive-ulcerative form
The most severe manifestation. Ulcers that do not heal for a long time form on the mucous membrane. This erosive-ulcerative form requires active medical intervention, as the risk of secondary infection and complications is highest.
Atrophic form
With this form, the oral mucosa becomes thinner. It appears varnished and bright red. Patients complain that it is painful to eat even familiar foods, let alone seasonings.
Hyperkeratotic form
Characterized by pronounced keratinization. The lesions become hard, dry, and may resemble calluses. This is common in long-term smokers.
The main preventative measures are:
- Oral self-examination in a mirror once a month
- Timely dental treatment and prosthetics
- Quitting smoking and spicy foods
- Get adequate sleep, minimize stress, and treat chronic gastrointestinal diseases
The main goal is to boost immunity.
FAQ
Is it possible to permanently cure oral lichen planus?
Is this disease contagious among family members?
Should all crowns be removed if ringworm is detected?
Oral lichen planus is always a sign of immune system problems. The key is not to panic or self-medicate. Early diagnosis of oral lichen planus, elimination of the underlying factors, and appropriate therapy are key to quickly resolving the problem.

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Price
























































































What is oral lichen planus?
Lichen planus (LP) is a disease of the skin and mucous membranes. Painful rashes (ulcers) appear in the mouth.
It is not infectious: it is not transmitted through kissing, sharing utensils, or household contact. A person becomes ill due to a weakened immune system: their body's cells begin to attack the mucous membrane epithelium.
Which areas of the mucous membrane are most often affected?
The pathological process is most often localized on the mucous membrane of the cheeks, especially in the posterior areas, closer to the molars. Lesions are also often found on the lateral surfaces of the tongue, gums, and, much less frequently, on the lips or palate. A characteristic feature of LP is its symmetry: if the characteristic white streaks on the oral mucosa appear on the right side, they are highly likely to appear on the left side as well.
How does it differ from stomatitis and other inflammations of the mucous membrane?
Unlike common aphthous stomatitis, which resolves within 7-10 days, lichen planus in the mouth is persistent. Stomatitis typically appears as a single, painful ulcer with surrounding redness, while lichen planus often presents as a network of whitish lines (Wickham's grid) that do not come off with a spatula. This is an important difference from candidiasis (thrush), where the white coating is easily removed, revealing reddened tissue.
The disease requires long-term observation, as it tends to have an intermittent course with periods of remission and exacerbations.