Lumbar Disc Herniation
A lumbar disc herniation is a bulging disc. The disc loses its strength. Some of its tissue shifts beyond its normal contour, sometimes toward the spinal canal.

specialists

equipment

treatment
Symptoms
Symptoms of this condition depend on the location of the hernia. They also depend on the extent of its impact, that is, the pressure it places on the nerve root or spinal canal. The most common scenarios include lower back pain radiating to the arm, leg, or buttock. The pain intensifies when bending over or coughing. Pain can also occur after prolonged sitting. Some patients complain of a tingling sensation, decreased sensation, and weakness in the foot. Such complaints are usually considered to indicate significant nerve root compression.
Important: if any "red flag" symptoms appear, do not delay – the doctor will assess the neurological status and determine whether urgent surgical intervention is required.
A quick tip: it's not just the severity of the pain that's alarming, but also the persistent impairment of function.
- Lumbar pain that worsens with exertion
- Pain radiating along the nerve to the thigh/calf
- Numbness, tingling, decreased sensation
- Muscle weakness, buckling of the leg, changes in gait
- Limited movement, forced posture
- In severe cases – urinary problems and severe weakness (reason for urgent medical attention)
Reasons for occurrence
The process of disc herniation is lengthy. It begins with the disc aging and losing moisture, making it less elastic. Pressure within the segment is less well distributed, so the lower back begins to pay for any physical activity, whether walking, bending, carrying heavy objects, or working in a static position. Then comes the moment of breakdown. This can be a sudden movement or a prolonged load, or even lifting with improper technique. As a result, the fibrous ring ruptures, causing a portion of the disc to protrude beyond its normal contour. Sometimes, trauma is the trigger. In this case, cumulative factors are triggered, including weak muscular corset, lack of stabilization, and a habit of overloading the lumbosacral region.
The appearance of a herniated disc is not a reason for surgery, and there is no need to worry too much, as it is not a death sentence. In the earliest stages, conservative therapy is appropriate. In this case, medications are prescribed according to the doctor's instructions, a gentle regimen, and low-stress lumbar spine exercises are recommended. Rehabilitation then follows, and if successful, the problem is resolved. The patient regains full range of motion, and the muscular corset is significantly strengthened.
If the pain recurs or intensifies, don't wait until the discomfort becomes critical: early diagnosis and treatment selection reduce the risk of complications and increase the chances of avoiding intervention.

- Prolonged sedentary work and weak core muscles
- Excessive physical activity or lifting heavy objects with a straight back
- Excess weight, which increases pressure on the lumbar spine
- Congenital spinal structural abnormalities and segmental instability
- Previous injuries, especially at the L4-L5 or L5-S1 (sacral segment) level
- Age-related changes in the disc and deterioration of its nutrition
Indications for surgery
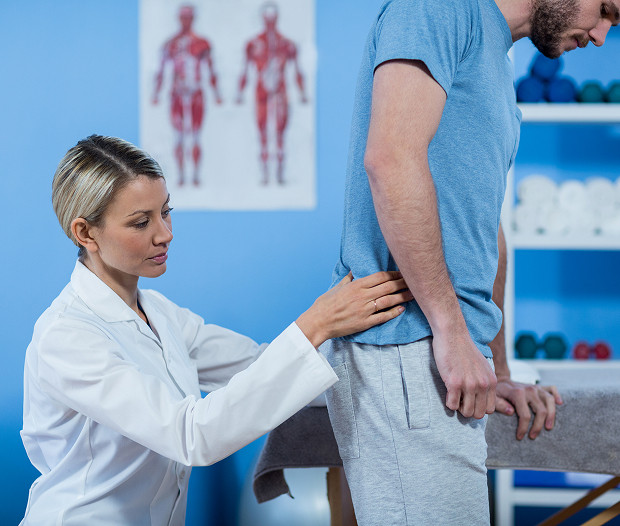
The decision to operate is made when symptoms interfere with life or there is a risk of persistent neurological disorders. Lumbar disc herniation is considered not "based on the x-ray," but based on clinical findings: how severe the pain is, how the patient responds to treatment, and whether there is progression of weakness and sensory disturbances.
In most cases, conservative treatment is tried first, but with certain symptoms, waiting is dangerous.
- Persistent, severe pain that does not respond to therapy and rehabilitation
- Progressive weakness, decreased muscle strength at a specific level
- Signs of severe nerve root compression according to MRI data, combined with symptoms
- Signs of compression of the canal structures with the risk of complications
- Repeated exacerbations that severely limit the patient's activity
- "Cauda equina" syndrome (emergency indication)
After this, the doctor discusses the method: microsurgical, endoscopic, or another option, and It also explains how the surgery will be performed and what kind of rehabilitation is needed.
Contraindications to surgery

Contraindications can be temporary or permanent: sometimes the procedure is postponed to reduce risks, while other times an alternative approach is chosen. The important goal is patient safety and a predictable outcome.
- Acute infections, high fever, active inflammation
- Decompensation of chronic diseases, unstable blood pressure
- Bleeding disorders without correction
- Severe conditions in which the risks of anesthesia outweigh the benefits
- Pregnancy (an individual decision; surgery is often postponed)
When contraindications are temporary, the doctor prescribes preparation for surgical planning. This means that if there are contraindications, the patient's general condition is first stabilized, blood pressure is normalized, any infections are treated, and blood counts are adjusted. Only then is the patient cleared for surgery. This approach reduces the risks of anesthesia, as well as postoperative complications.
Why is it better to have a lumbar disc herniated at the K+31 clinic?
When choosing a location for lumbar disc herniation, the team's experience, diagnostics, and a convenient patient journey are important. K+31 offers a multidisciplinary approach: you can undergo examinations, receive consultations, and plan your rehabilitation in one center, and the booking and service navigation are clearly organized. This reduces the "gap" between diagnosis, surgery, and recovery—especially important when pain limits movement and time is critical.


This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Price
Other services







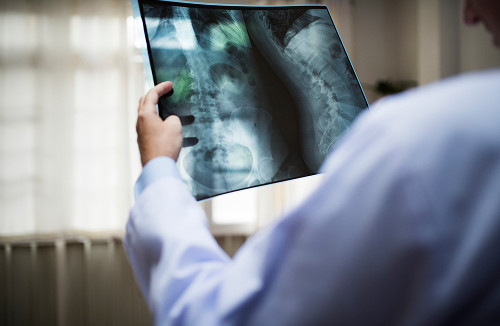



























































































What is a lumbar disc herniation?
A lumbar herniated disc is a bulging disc. The disc loses its strength. Some of its tissue shifts beyond its normal contour, sometimes toward the spinal canal.
The lower back suffers, as does the lumbosacral region. This is where the greatest strain occurs. Walking, bending, and heavy lifting are common. The vertebrae in this area work hard and every day, so the intervertebral disc wears out faster and bulges more easily.
If the herniated disc compresses nerve structures, the picture changes. Radicular pain appears. Numbness develops. Sensation decreases. Weakness in the leg may occur. In these cases, treatment is not limited to pills. Rehabilitation is necessary. And in cases of severe compression or persistent neurological deficit, surgery may be required.
A herniated disc manifests differently in different people. This is crucial. One patient's complaints are minimal—episodic pain, no neurological deficit, and symptoms persist despite therapy and rehabilitation. Another's progression is more rapid: the pain becomes constant, intensifies with movement, and numbness, decreased sensation, and weakness in the leg develop, all signs of nerve root compression. Therefore, the question of whether a herniated disc needs to be removed is decided on a case-by-case basis. During an in-person appointment, after an examination and clinical assessment.