Gastrostomy Tube Placement in Palliative Care: What Patients and Their Families Need to Know
When a person is seriously ill, one of the most pressing issues for families is nutrition. Some people stop swallowing, others choke even on water, and still others simply eat everything but can't gain weight. Gastrostomy tube placement is a procedure that addresses these issues: it reduces the risk of choking, and feeding becomes a routine rather than a complicated process.

specialists

equipment

treatment
Indications for the procedure: when is it time to think about gastrostomy?
The decision is always made by a doctor, but a gastrostomy is usually placed when oral feeding is impossible. This is especially important in situations where the patient is rapidly losing weight, and attempts to feed them even a little food result in vomiting or choking.
Swallowing difficulty (Dysphagia)
Dysphagia is when a person chokes, coughs, or swallows saliva. If food gets into the wrong throat, the patient can simply choke. But even without considering the most tragic outcome, aspiration pneumonia can occur.
A gastrostomy for a bedridden patient in such cases is much better than a feeding tube because it reduces the risk of aspiration compared to a nasogastric tube.
Inability to adequately eat orally
Many patients can swallow, but due to severe weakness, spread of metastases, or nausea, they are unable to eat normally. Systemic malnutrition is a direct path to dramatic weight loss. In this case, the body simply has no strength left to fight the disease: wounds heal more slowly, and muscle and joint pain increases.
A gastrostomy tube for oncology is a way to support the body and enable a person to live a normal life.
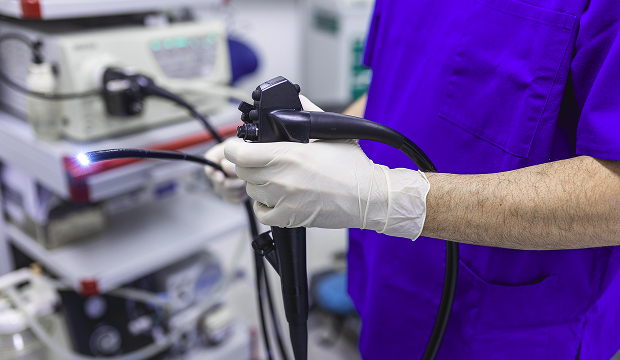
Types of gastrostomy: why is PEG (endoscopy) better?
Endoscopic gastrostomy (PEG, percutaneous endoscopic gastrostomy) is a way to place a feeding tube directly into the stomach without a full-blown operation. The doctor performs this procedure using an endoscope: a thin, flexible tube with a camera is inserted through the mouth, the stomach is examined from the inside, and the gastrostomy tube is precisely positioned.
This option is usually easier to tolerate because it is less traumatic, and recovery is quicker. For long-term feeding, this is generally a convenient solution. In some cases, the doctor may choose a Pezzer catheter, depending on the patient's condition, diagnosis, and overall treatment plan.
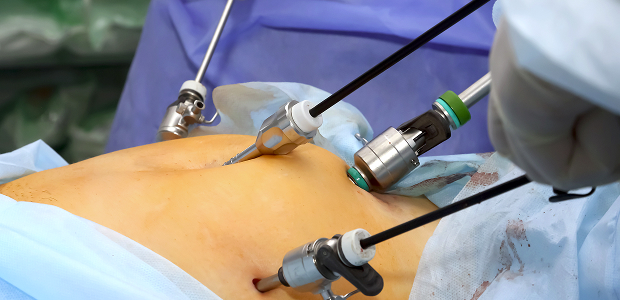
How the installation process works: stages and preparation
First, the patient is examined, risks are assessed, and tests are completed. Then, the surgery is performed. General anesthesia is not required; sedation or local anesthesia is used.
After the tube is inserted and secured, the doctor explains basic care to the patient and their family. They also explain how to feed with the tube, how to care for the wound, and what symptoms require calling a doctor.
Life and care after the procedure
Gastrostomy placement is a procedure that simplifies patient care and makes life more comfortable for the patient and their family. Fear is alleviated for relatives, and panic is eliminated for the patient. They no longer fear that any careless movement could result in choking or vomiting.
But for everything to go smoothly, it's important to learn how to properly care for the stoma. The doctor will explain everything during the consultation, but relatives must strictly follow their recommendations, without any self-initiated efforts.
Hygiene rules around the stoma
The patient's family should monitor the gastrostomy opening. This should be done daily: the wound should be dry, free of redness, odor, and pain. Simple care: treat it with an antiseptic twice a day, but the doctor will provide more precise recommendations.
Small granulations are common, but if they grow, bleed, or become wet, this is a reason to consult a doctor to prevent a stoma infection.
Features of the introduction of nutrition and medications
Feeding through a gastrostomy is introduced gradually. It is not necessary to administer the full daily volume from the very beginning.
Feeding formulas are usually used. The consistency, volume, and content are determined by the doctor.
Particular attention should be paid to taking pills. People with swallowing difficulties cannot take medications orally. These are also administered through the gastrostomy, but it is important to note that not all pills can be crushed. Therefore, it is not possible to add or stop medications on your own: the dosage and administration format are determined by the doctor.
After each administration, the system is flushed to reduce the risk of blockage. And no matter what you administered—food or medication—the stoma must be clean.
Prevention of complications
What problems can arise when feeding through a gastrostomy tube? Most common problems include leakage of stomach contents, skin irritation, tube blockage, and infection. To prevent these problems, always flush the stoma and secure it without tension on the skin.
If you experience pain, fever, purulent discharge, or a strong odor, consult a doctor immediately.
Psychological aspect: how to make a decision?

People often fear that a gastrostomy is a "point of no return." In practice, palliative care gastrostomy is often about freedom: the patient suffers less, and the family no longer lives in constant fear of aspiration.
Sometimes it's helpful to ask yourself a simple question: what's more important now—continuing to struggle with every spoonful or providing the body with nutrition safely?
Table: Tube or gastrostomy
| Parameter | Nasal tube | Gastrostomy |
|---|---|---|
| Duration | Short-term (up to 4 weeks) | Long-term (6–12 months and longer depending on the situation) |
| Comfort | Discomfort in Nasopharynx, may prolapse | In the stomach, usually barely felt |
| Aesthetics | Visible on the face | Hidden under clothing |
| Risk of injury | Higher (nose, esophagus) | Low with proper care |
| Risk of aspiration | Increased | Decreased |
| Care | Often more difficult Keep in place | Requires skin care, but is stable |
Conclusion
Gastrostomy placement solves more than just nutritional issues. This procedure simplifies patient care and allows families to live their lives free from fear, constant panic, and insomnia.
Gastrostomy placement for oncology patients is the best way to maintain strength and reduce the risk of aspiration.
We provide a full cycle of support: from safe placement to educating the family on how to cope with the new circumstances.

FAQ
Is the implantation procedure painful?
Can I continue eating orally after a tube is inserted?
How often should the tube itself be changed?
Is a gastrostomy tube visible under clothing?
Is a gastrostomy permanent for a bedridden patient?
How is a PEG tube better than a standard tube?
When should you see a doctor?
Important: This article is for informational purposes only. Only a doctor can make all decisions. You should not change your diet, consistency, or volume on your own.
Our doctors

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Other services









































What is a gastrostomy and why is it needed?
A gastrostomy is an opening (essentially a controlled fistula) through which a feeding tube is inserted into the stomach. It's practically invisible under clothing, so there's no need to worry about your loved one's appearance or self-esteem.
The main goal is nutritional support. The primary task facing relatives and palliative care physicians is to ensure the person receives their daily calorie intake. In other words, you don't need to feed them at any cost, but rather help the body cope with the disease.