Hepatocellular Carcinoma: How Palliative Care Helps
Hepatocellular carcinoma is a liver cancer that develops from hepatocytes. In its late stages, the disease affects not only the liver but the entire body. The patient experiences weakness, sleep disturbances, loss of appetite, and mood swings. The family feels helpless. They don't know what to do, how to help, or how to relieve pain. Palliative care physicians answer these questions.
Contrary to popular belief, palliative care is not a refusal of treatment; it is a change of direction. If the disease cannot be cured, then a decent quality of life must be ensured.

specialists

equipment

treatment
Objectives of palliative care in liver cancer

Liver cancer and palliative care are a complex process aimed at pain relief, nutritional support, and family support.
In the later stages, palliative treatment for liver cancer is often carried out in parallel with anticancer therapy:
- The doctor prescribes targeted medications (targeted at eliminating a specific problem)
- Immune medications are added
- Consultations with other doctors are scheduled
Palliative care is a team effort. Nurses care for the patient, doctors prescribe treatment, and a psychologist helps cope with depression.
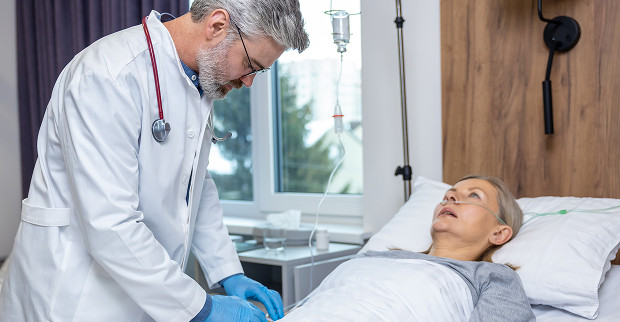
Pain Management
Pain from liver damage can vary: dull and constant, intermittent, and sometimes radiating to the back or shoulder.
Pain management is based on a stepwise approach: mild analgesics are selected first, and stronger medications are added if necessary. It is important to take them on schedule, not when the pain is unbearable.
A person can only live a normal life if they get enough sleep and are in a healthy psychological state.
Main symptoms and methods of their relief
Symptoms of late-stage liver cancer typically include weakness, weight loss, nausea, itching, jaundice, and abdominal distension due to fluid retention. These symptoms can be frightening, but many can be alleviated with systematic intervention.
Combating Ascites and Edema
Ascites in liver cancer is a buildup of fluid in the abdomen. The patient's abdomen swells, the intestines swell, and bowel movements become irregular.
The doctor prescribes diuretics and monitors fluid intake. If all else fails, surgeons drain the fluid: this is the only way to return to normal life.
Nutrition status correction (nutrition)
Hepatocellular carcinoma wreaks havoc on the body. A person eats little, quickly loses weight, and loses strength. If nutritional support is insufficient, high-protein foods—nutrition shakes—must be introduced.
Important: This diet should be prescribed by a doctor. They will explain how and in what quantities to take it. The most common regimen is 5-6 small meals a day. Your goal is to provide the body with the necessary vitamins and not overfeed. This impacts the patient's quality of life, because strength means the ability to get up, talk, and be with loved ones.
Psychological Support for Patients and Family
Late-stage cancer almost always brings anxiety and a feeling of loss of control. Patients fear pain, and families fear they won't be able to cope.
Psychological support helps reduce stress, restore sleep, and foster conflict-free conversations within the family. Sometimes this is enough to make everyone feel better—even physically.

Caring for a cancer patient at home is possible if the patient's condition is relatively stable and there is contact with a doctor. The key is simple organization: a comfortable bed, everything needed nearby, and a symptom diary (pain on a scale of 0-10, appetite, stool, temperature, and swelling severity). This helps the doctor adjust symptomatic therapy more quickly.
Maintain safety: prevent falls, practice good skin hygiene, and monitor bowel movements (constipation increases toxicity). If encephalopathy worsens, it's important not to argue or "educate" the patient, but rather to provide a calm environment and consult a doctor—sometimes detoxification and a review of therapy are necessary.
If it's difficult for the family to provide 24/7 care, they can arrange for home care, and sometimes the best option is to temporarily move to a hospice, which offers 24/7 monitoring and support for the family.
Table: Active treatment and palliative approach
| Parameter | Active treatment | Palliative approach |
|---|---|---|
| Goal | Contain tumor, prolong life | Comfort, symptom control |
| Methods | Targeted therapy, immunotherapy, procedures according to indications | Pain management, detoxification, nutritional support, care |
| Expected outcome | Slowing progression | Improving well-being and quality of life |
| Psychological aspect | Stress of anticipating the effect | Focus on calm and family support |
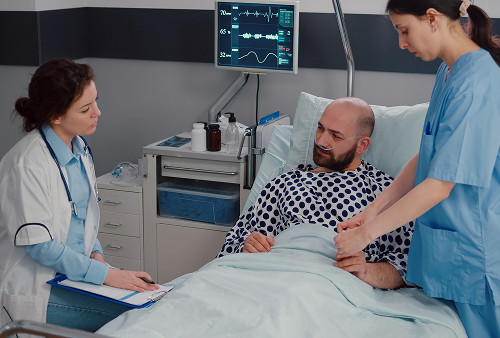
Conclusion: Life without pain is possible

Advanced hepatocellular carcinoma is a difficult ordeal, but that doesn't mean a person has to suffer. Palliative care for liver cancer and palliative treatment for HCC can help control pain, reduce ascites, maintain nutrition, and preserve dignity.
A patient's quality of life depends on simple things: being pain-free, being able to sleep, eat, and talk. And this is truly achievable.
Frequently Asked Questions
How do you know when your pain medication needs to be changed?
What should you do if ascites worsens and breathing becomes difficult?
Will nutrition help if you have almost no appetite?
Our doctors

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Other services









































Features of the disease in the late stages
Hepatocellular carcinoma often develops against a background of chronic liver problems, so the symptoms are divided into two layers: those of cancer and those of liver failure.
Bilirubin levels rise, toxicity intensifies, and encephalopathy may develop—confusion, drowsiness, and behavioral changes.
It's important to understand: deterioration can be intermittent. One day a person may look fine, but the next, they may feel worse.