Palliative Care in Oncology: When Medicine Cares About Quality of Life
Palliative care in oncology is frightening. But it's important to understand that palliative care doesn't mean refusing treatment; it's a transition to a different level of care.
While radical therapy aims to destroy the tumor, palliative care helps patients live without severe pain, shortness of breath, nausea, and fear. It's important for physicians to maintain patients' quality of life, even if the disease progresses.
This is especially true when it comes to helping stage 4 cancer patients. In this situation, medicine doesn't "give up." It changes its focus: we don't just treat the disease; we care for the person.

specialists

equipment

treatment
The main objectives of palliative care
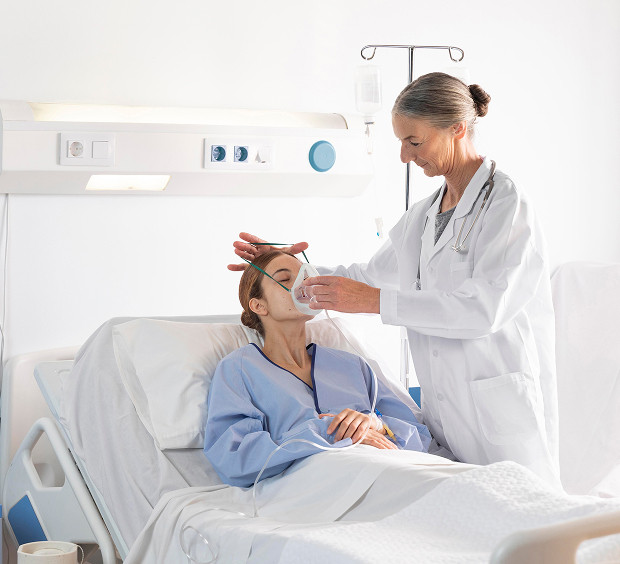
A palliative care oncologist is not a "doctor of last resort." They are a quality-of-life specialist. When a disease cannot be cured, the emphasis is on the patient's quality of life.
Pain and Physical Symptom Management
Pain is the most problematic factor. Pain management for cancer patients is the ability to control even severe pain.
Step therapy regimens, drug combinations, and, if necessary, opioid analgesics are used. Pain medications should be strictly prescribed by a doctor. Do not self-medicate if you have severe pain.
Modern symptom management methods are used in our practice: transdermal systems (patches), pain relief pumps, and modern pain medications.
In addition to pain, nausea, constipation, shortness of breath, and delirium are treated. This is symptomatic therapy.
Properly organized palliative care for oncology can reduce the intensity of symptoms and maintain the patient's activity.

Psychological Support for the Patient and Their Family
Cancer causes suffering for both the patient and their family. And it's not just the pain—palliative care also assesses the patient's psychological state.
A palliative oncologist can work with a psychologist. A poor prognosis, fear of death, guilt, and fatigue all require attention. Support for relatives of cancer patients reduces anxiety. A loved one's hospital stay is not an indicator of irresponsibility. It offers an opportunity to live a full life, work, get enough sleep, and come to their sick relative in a good mood.
Plans, expectations, and possible complications are discussed with a psychologist. No intimidation, just the facts.
It's important to understand that palliative care does not hasten death, but rather makes life as fulfilling as possible.
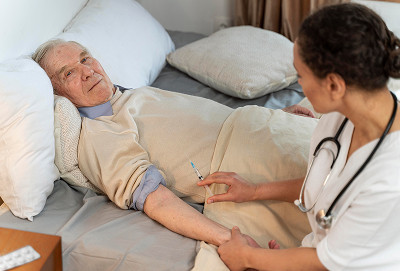
You should consult a palliative oncologist if:
- Pain persists despite treatment
- The patient refuses to eat due to nausea or weakness
- Severe shortness of breath, anxiety, or insomnia have developed
- This is for patients with stage 4 cancer and requires symptom control.
There's no need to wait until the "last resort." Palliative care can be used in conjunction with anticancer therapy.
Formats of assistance
Inpatient Unit
Suitable for severe conditions requiring 24/7 monitoring. Cancer pain management regimens are adjusted, dosages are adjusted, and side effects are monitored.
Mobile Palliative Care Service
A doctor and nurse come to the patient's home. This is convenient for patients with limited mobility. This maintains a stable quality of life for patients without unnecessary hospitalizations.
Hospice Care: Myths and Reality
Hospice is not a "waiting place." It is specialized palliative care for oncology patients, providing pain relief, care, and family support.
Here's the difference between radical treatment and a palliative approach:
| Parameter | Radical Treatment | Palliative Care |
|---|---|---|
| Goal | Complete Cure or Remission | Improved Quality of Life |
| Focus | Tumor Control | Symptom Control (Pain, Nausea) |
| Objective | Only Patient | Patient and Family |
How to prepare for a consultation: advice for relatives
Remember: the doctor's job is to prescribe medications and develop a clear plan for psychological and medical care.
- Monitor your symptoms and the frequency of pain increases. Your doctor will need this information to increase or decrease medication doses
- Have any prescriptions you already have on hand. The doctor needs to know what the patient is taking
- Talk to your sick relative. Learn about their fears and concerns, and be sure to share them during the consultation
- Always ask directly about the prognosis
Frequently Asked Questions
Is it possible to combine palliative care and chemotherapy?
Is the prescribed pain medication addictive?
Is it possible to receive official care at home?
Our doctors

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Other services











































Who is a palliative oncologist and what is their role?
A palliative oncologist helps the patient and their family. They assess pain, shortness of breath, weakness, sleep disturbances, and anxiety. They select a pain management regimen, monitor progress, and explain the patient's progress to the family.
The doctor develops a personalized plan to support the patient's well-being: from pain management to psychological support for the entire family.