Palliative care for rectal cancer: how to improve quality of life
When cancer reaches its final stage, relatives of the patient begin to wonder what will happen next. It's important to answer this question honestly: rectal cancer is a disease that requires palliative care. This isn't about giving up the fight. It's about changing your goal. We're no longer trying to defeat the tumor at any cost; we're trying to eliminate pain, reduce suffering, and preserve human dignity.
We need to treat not only the disease, but also the person, specifically their mental state. The fewer negative thoughts, the more opportunities there are to spend peaceful time with family.

specialists

equipment

treatment
Main symptoms and ways to relieve them
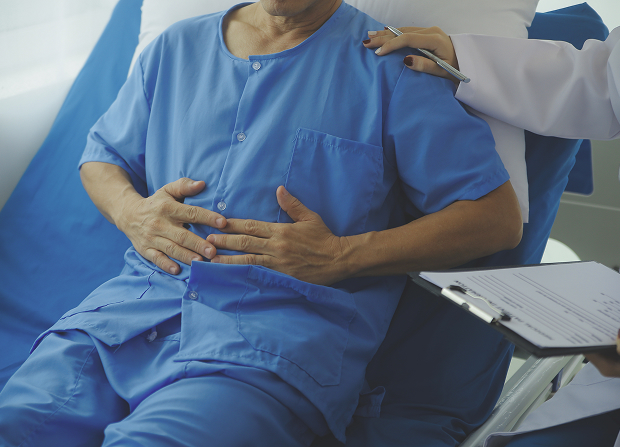
Symptoms of late-stage rectal cancer include bloody discharge, weakness, constipation, or diarrhea. Sometimes intestinal obstruction develops, and intoxication increases.
Each symptom requires an individual approach, and there's no need to tolerate them.
Pain therapy
Pain is assessed using a special scale to help determine the correct dosage.
Pain relief is gradual: from non-narcotic medications to stronger analgesics if needed. This principle applies, starting with lesser pain and progressing to greater pain relief.
Pain relief is not only part of palliative care. It is, above all, an opportunity to live a full life. The patient can spend time with family, sleep pain-free, and spend time the way they want to at that moment.

Correction of bowel function and fight against intoxication
Bow stool problems are a common problem. For constipation, laxatives are prescribed, while for diarrhea, dietary modifications and constipating medications are recommended.
If there is an intestinal obstruction, the doctor may decide to create a stoma.
When bowel problems occur, the body poisons itself. The patient becomes nauseous, weak, and unwilling to eat. If this occurs, infusion therapy and nutritional support should be initiated.
Patient care features
Care for colorectal cancer requires a systematic approach. Families need to understand that life will never be the same. Every day is a struggle with fear and pain. If you feel you're overwhelmed, don't be embarrassed: call a palliative care physician and ask for support.
Caring for your stoma (if installed)
If a stoma has been created, it's important to choose the right ostomy pouches—based on size, type of attachment, and skin sensitivity. Modern systems are leak-proof and comfortable, reducing the risk of leakage and irritation. It's best to inspect the skin around the stoma daily: redness, oozing, itching, or pain are reasons to avoid putting up with them; consult a nurse or doctor. When changing the pouch, wash the skin with warm water without harsh soap and dry thoroughly to ensure the adhesive adheres securely. If you're prone to irritation, protective pastes and wipes can help—they're individually selected to ensure calm and predictable care for rectal cancer patients.
Organization of food and hygiene
Meals should be small and gentle. Soft or pureed foods should be consumed. Nutritional support helps maintain strength, but such drinks should be introduced gradually: monitor the child's response, weight, and stool.
Moisture-absorbing underwear, anti-decubitus systems, and proper body positioning reduce the risk of pressure ulcers.
Psychological support for the family
Oncology is almost always associated with depression. No matter what stage the patient is in, their psychological state can worsen with each passing day.
The family of a cancer patient also faces a difficult situation: relatives fear the future, and they fear the patient's suffering.
Psychologists can help cope with this situation. They help the patient survive this stage and regain their footing. Both the patient and their family need to understand how to ask for help and how to discuss difficult topics without conflict.
Often, such conversations can even lead to physical relief: sleep improves, stress decreases, and compliance with treatment and care is easier. Support from relatives reduces emotional burnout and guilt, which can greatly interfere with life. And most importantly, it helps the family remain a family, rather than turning into a 24-hour shift of caregivers.
When is it necessary to contact a palliative care unit?
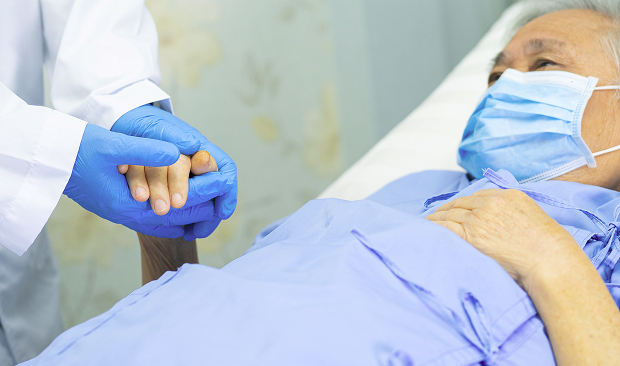
Contacting a palliative care unit should be considered if it becomes difficult to manage the situation at home. The first sign is when the pain no longer responds to the prescribed treatment and requires increasingly frequent "catch-up" treatments, which disrupts sleep and appetite. The second sign is increasing weakness, making it difficult for the person to get up, eat, or go to the toilet, and caring for the family takes up almost the entire day. The third sign is complications: severe intoxication, signs of intestinal obstruction, dehydration, frequent infections, and the development of pressure ulcers. Inpatient care or hospice care offers 24-hour monitoring and the ability to quickly adjust therapy, as well as professional nursing care. Importantly, hospice care is not a "last resort," but a way to stabilize the condition and relieve the family of some of the burden, so that loved ones can be with them calmly, rather than at the end of their tether.
Table: home care vs. Inpatient palliative care unit
| Parameter | At home | In the unit |
|---|---|---|
| Pain management | As prescribed by a physician | 24-hour monitoring |
| Hygiene | Family efforts | Professional care |
| Equipment | Purchased separately | Provided |
| Psychological support | Upon request | As part of a team |
| Rehabilitation | Limited | Under the supervision of specialists |
Conclusion
Colorectal cancer and palliative care are a professional approach to living pain-free. It's not about giving up the fight, but about fighting for a dignified life, even if the disease progresses.
A comprehensive approach—from medical procedures to spiritual and psychological support for the entire family—helps maintain respect for the individual and their right to comfort.

FAQ
Is it possible to relieve pain at home for stage 4 cancer?
What should you do if a patient refuses to eat?
How can I care for my stoma myself?
How does palliative care differ from hospice?
Is it possible to completely eliminate pain?
Is hospitalization always necessary?
Is home care feasible?
Our doctors

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Other services









































Objectives of the palliative approach in late-stage cancer
When palliative care is established, pain control and complication prevention become top priorities.
Rectal cancer and palliative care are all about pain relief. The doctor not only focuses on treating the underlying disease but also tries to address problems associated with gastrointestinal dysfunction.
Palliative care also includes psychological support, proper diet planning, and pressure ulcer prevention.
Even if the diagnosis is terminal, the goal remains the same: helping the patient live without excruciating pain and debilitating thoughts.