Inpatient Stroke Treatment: From Intensive Care to Recovery
A stroke is an acute cerebrovascular accident. Yes, there are mild forms, when a person doesn't even notice any changes. They may have a severe headache or a burst blood vessel in the eye. But even in these cases, every hour counts: the sooner the patient gets to the hospital, the better the chance of preserving speech and facial and body muscle mobility.
Inpatient stroke treatment is the only way to reduce the consequences of the disease. Doctors will immediately take tests, perform an MRI, and begin treatment. After the dangerous symptoms have subsided, stroke rehabilitation begins in the hospital with a team of specialists.

specialists

equipment

treatment
Stages of patient treatment in hospital

Immediately upon admission, the patient is examined by a neurologist. Their pulse, blood pressure, and oxygen saturation are measured. After this, they are immediately referred for an MRI or CT scan.
Treatment is then prescribed. This depends not only on the type of stroke but also on the patient's condition: those in critical condition are sent to the intensive care unit, while those in more or less stable condition are transferred to the neurology department.
Specialized Neurology Department
When the patient recovers, they are transferred to the neurology department. Here, treatment continues and early rehabilitation begins: standing, exercise therapy, and assessment of swallowing, speech, and memory.
The department physician develops an action plan for restoring mobility. Even if a person can move and speak after intensive care, this does not mean they can get out of bed. All actions are coordinated with a neurologist.
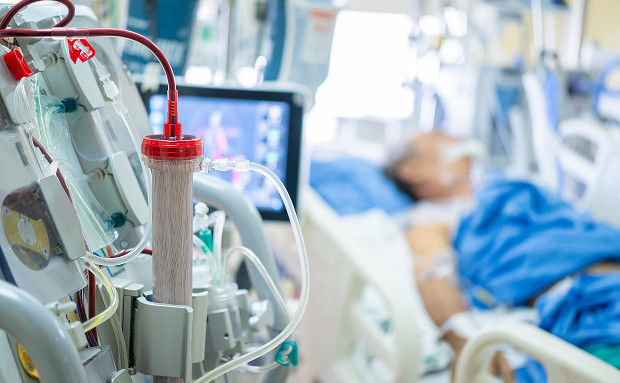
Intensive Care and Resuscitation
Not all patients require intensive care. Typically, patients with high blood pressure that can't be controlled with standard medications, as well as those with seizures and low oxygen saturation, are admitted there.
Why intensive care? Doctors in this unit monitor the patient's condition throughout the day. Patients are connected to monitors, allowing them to monitor their blood pressure, pulse, and heart rate around the clock.
It's important to understand: intensive care is a bad sign. Don't prepare yourself for the worst. This is an opportunity to recover from a stroke without any complications. A person in this unit is safe.
Inpatient Treatment Methods
Treatment depends on the type of stroke and the condition of the blood vessels. All medications and procedures are prescribed based on test results and MRI.
In ischemia, the main goal is to restore blood flow; in hemorrhage, the goal is to stop the spread of damage and mitigate the consequences of the incident.
Drug Therapy and Thrombolysis
For ischemic stroke, treatment includes blood pressure control, clot prevention, risk factor correction, and metabolic and respiratory support. In some patients, thrombolytic therapy may be administered within the first 4.5 hours in an attempt to dissolve the clot and restore blood flow to the affected vessel.
Important: Thrombolysis should not be performed without CT/MRI, as it is dangerous in hemorrhagic stroke.
Surgical Treatments, If Necessary
In the case of a hemorrhagic stroke or certain complications, neurosurgical interventions may be necessary:
- Hematoma Removal
- Bleeding Control
- Vascular Surgeries
The decision is made jointly by a neurologist and neurosurgeon, based on the location of the hemorrhage and the patient's condition.
Most often, after surgery, the patient is admitted to the intensive care unit. This does not mean that their condition has worsened; doctors simply need to increase monitoring. If there are no problems the next day, the patient is transferred to the neurology department.
Table: Ischemic and Hemorrhagic Stroke
| Stroke Type | Treatment Principle |
|---|---|
| Ischemic | Restoration of blood flow (thrombolysis if indicated), clot prevention, blood pressure control |
| Hemorrhagic | Bleeding control, neurosurgery if indicated, strict blood pressure control |

Early Rehabilitation in a Hospital Setting
Rehabilitation begins in the hospital. It is necessary for all patients without exception, and this stage cannot be ignored.
The rehabilitation therapist's goal is to activate neuroplasticity. The patient's brain must learn to live in a new reality and restore lost functions.
In the department, doctors focus on:
- Preventing bedsores and contractures
- Monitoring blood pressure and temperature
- Monitoring the condition of the oral mucosa and skin
- Assisting people with limited facial muscle movement to eat and drink
Restoring motor functions and physical therapy
Physical therapy begins with the simple: correct body position, simple (slow) movements, getting out of bed, and steps with support.
At the same time, they work on balance and fall prevention. This can help you overcome temporary paralysis more quickly and return to normal life (at least to self-care).
Working with a Speech Therapist and Neuropsychologist
If speech is affected, a speech therapist is involved: restoring articulation, swallowing, and speech comprehension. A neuropsychologist works with memory, attention, behavior, and reduces anxiety. This part of rehabilitation often determines whether a person can communicate and live without constant assistance.
Frequently Asked Questions
Is it possible to treat a stroke at home if you're feeling a little better?
Why does everyone get a CT or MRI scan right away?
What should relatives do in the first 24 hours?
Our doctors

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Other services
















































Why is urgent hospitalization important for stroke?
Stroke cannot be treated at home. Simply waiting, lying down, or taking a blood pressure pill won't do. To begin treatment, it's important to determine the exact type of stroke. This is done by performing a tomography (CT/MRI) scan.
After receiving the images, the doctor makes a precise diagnosis: ischemic or hemorrhagic.
The Golden Hour Rule
The first few hours are especially crucial. Before severe brain damage occurs, a person has a chance for a full life. The longer you delay hospitalization, the more severe the damage.
Treatment for ischemic stroke is aimed at reversing the consequences of the disease. Doctors strive above all to ensure a normal quality of life: they need to preserve speech and movement.
If treatment is delayed, the patient may develop paralysis. Therefore, thrombolytic therapy should be administered within the first 4.5 hours from the onset of stroke symptoms.