Comprehensive in-patient treatment of varicose vein complications: from thrombophlebitis to trophic ulcers
Varicose veins of the lower extremities are more than just an aesthetic problem. In the late stages of the disease (according to the international CEAP classification, these are levels C4–C6), serious tissue changes occur. Venous outflow decompensation develops, leading to vein inflammation and the formation of open wounds. In-patient treatment of varicose veins is the only way to stop the progression of the disease and avoid disability.
A comprehensive approach in a specialized department allows for the healing of trophic ulcers and the elimination of the cause of varicose veins in a single hospitalization. This is achieved through the coordinated work of a team that includes not only a vascular surgeon and phlebologist, but also a physiotherapist, cardiologist, and rehabilitation specialists.

specialists

equipment

treatment
Treatment of thrombophlebitis in a hospital setting
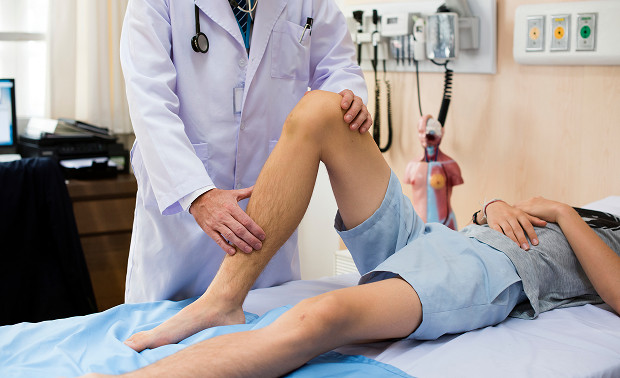
Acute thrombophlebitis is an inflammation of the saphenous vein wall, accompanied by the formation of a thrombus within its lumen. The main danger here is the potential for the process to spread to the deep veins and develop into pulmonary embolism (PE).
Conservative and Surgical Approaches
If the thrombus is located in the upper third of the thigh and threatens to spread to the common femoral vein, the vascular surgeon decides on emergency surgery. The classic method is the Troyanov-Meyers procedure (crossectomy)—ligation of the ostium of the great saphenous vein. Modern protocols allow this intervention to be combined with minimally invasive techniques to minimize tissue trauma.

Relief of Acute Inflammation and Prevention of Pulmonary Embolism
Inflammation is relieved with anticoagulants—medications that thin the blood and prevent clot growth. This is the same as thrombosis prevention. These medications are available by prescription, and the dosage must be prescribed by a doctor. In the hospital, the dosage is monitored with daily blood tests. This cannot be done at home.
Caution! Self-medication with ointments for thrombophlebitis is dangerous due to the risk of clot dislodgement. Massage and warming the legs during signs of vein inflammation are strictly contraindicated, as any thermal or mechanical stimulation can provoke clot migration through the bloodstream.
Therapy for trophic ulcers in varicose veins
Treating trophic leg ulcers is a lengthy process. It requires sterile conditions, which are simply impossible to create at home.
Ulcers develop when the vein valves stop working, blood stagnates, and tissue begins to die due to a lack of oxygen.
Stages of Wound Defect Cleansing and Healing
The inpatient recovery process is divided into stages:
- Cleansing of the trophic ulcer. Necrotic tissue and purulent plaque are removed. In the hospital, enzymatic preparations and special sorbents are used for this.
- Tissue granulation. When the wound is clean, new vessels and connective tissue begin to grow. This appears as a bright red, granular surface.
- Epithelialization. Covering the defect with skin. At this stage, protecting the young skin from damage is extremely important.
Modern Methods: Shave Therapy and EVLT
Today, leading clinics are abandoning the traumatic methods of the past (such as Babcock phlebectomy) in favor of technologies that can be used even on open wounds.
Endovenous laser coagulation (EVLT) is used. The laser seals the diseased vein from the inside. Eliminating the pathological blood flow is key to ulcer healing.
Shave therapy is also used. This is the surgical excision of the altered tissue at the base of the ulcer down to the healthy layers, which dramatically accelerates healing.
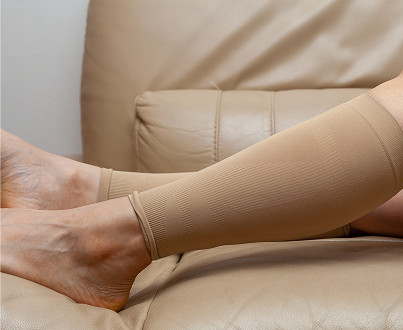
The Role of Compression Therapy in a Hospital Setting
Complicated varicose veins cannot be treated without external pressure on the veins. In hospital settings, special compression stockings or elastic bandages are used. This helps restore valve function and direct venous outflow into the deep system. A phlebologist selects the compression level individually, ensuring that the bandages do not compress the arteries.
Benefits of staying in hospital
Many patients fear hospitalization, but acute thrombophlebitis, treatment of which is initiated in the hospital, has the most favorable prognosis.
| Parameter | Outpatient treatment | Inpatient treatment |
|---|---|---|
| Blood clotting monitoring | Periodic, at the patient's responsibility | Daily, under strict physician supervision |
| Leg regimen | Necessity for movement and household chores | Strict rest or measured walking |
| Ulcer treatment | Self-treatment or infrequent dressing changes | Sterile dressing changes by a specialist 1–2 times a day |
| Treatment adjustments | Only during a follow-up visit to the doctor | Immediately, at the slightest change in condition |

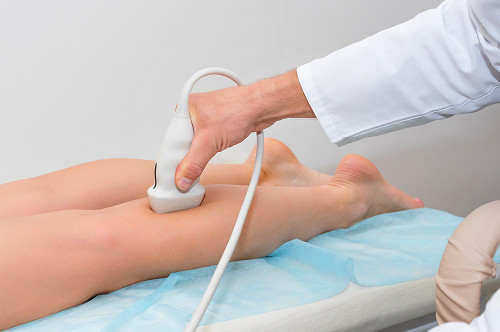
Before inpatient treatment for varicose veins, a standard diagnostic test is required.
To do this, you should consult a general practitioner, who will refer you for an ultrasound angiography (ultrasound angioscanning) of the veins. This procedure is necessary to determine the condition of the valves and the exact location of the blood clots.
You should also undergo coagulation tests (coagulogram), complete blood counts, urine tests, an ECG, and obtain a physician's report. If there is significant skin pigmentation or signs of eczema, a consultation with a dermatologist may be necessary.
Frequently Asked Questions
How long should I stay in the hospital?
Can laser surgery be performed if the ulcer hasn't healed yet?
Is it necessary to shave my legs before hospitalization?
Will treatment help if I already have dark spots (pigmentation) on my legs?
Our doctors

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Other services















































When outpatient treatment is not enough: indications for hospitalization
Treating chronic venous insufficiency (CVI) at home isn't the best option. Ointments and folk remedies won't just be effective, they can actually make things worse.
Hospitalization is necessary in the following cases:
Inpatient phlebology is the best way to return to a life free of pain and swelling.