Treatment of Meniere's disease
Ménière's disease is a disorder of the inner ear. It is chronic and intermittent. Clinically, it presents as sudden episodes of vertigo, tinnitus, and a feeling of pressure or fullness. Hearing function changes over time. The term "Ménière's syndrome" is used when symptoms are similar, although the cause is different—as a manifestation of a different pathological process. Two steps are then important: stop the attack and confirm the diagnosis. This helps us understand the underlying mechanism and the expected prognosis.

specialists

equipment

treatment
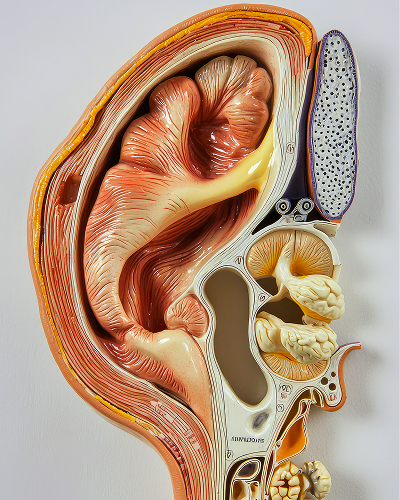
Etiology and pathogenesis
The primary mechanism of Ménière's disease is endolymphatic hydrops. Endolymph accumulates within the membranous labyrinth, increasing pressure in the inner ear structures. The vestibular system begins transmitting inconsistent signals, leading to vertigo. During an attack, hearing often decreases. Fluctuations are possible. In severe cases, repeated episodes disrupt the functioning of the sensory hair cells, and hearing loss becomes permanent.
There is no single mechanism for all patients. Ménière's disease develops according to different scenarios, and each person has their own set of triggers. Therefore, diagnostics are necessary to clarify the cause and identify the triggers that initiate an attack.
Causes
In clinical practice, several groups of causes are distinguished. Each of them has a different impact on endolymphatic flow and pressure in the labyrinth. For example:
- Dysregulation of endolymphatic outflow (endolymphatic sac and ducts)
- Vascular and metabolic factors affecting internal blood flow and nutrition
- Immune reactions that can maintain an inflammatory background
- Consequences of previous ear infections or injuries
After determining the cause, the doctor selects a treatment: from gentle regimens to procedures if conservative treatment fails to provide control.
Risk factors
There are conditions in which attacks occur more frequently and are more severe. Lifestyle and comorbidities influence endolymph balance and labyrinthine pressure. Therefore, the physician considers these factors when choosing a treatment plan and monitoring regimen.
In Ménière's disease, there are factors that increase the frequency of attacks and make them more severe. These factors are taken into account when choosing a treatment and monitoring regimen:
- Stress. Chronic sleep deprivation.
- Fluctuations in blood pressure. Shifts in fluid and electrolyte balance that affect fluid regulation in the inner ear.
- Excess salt in the diet.
- Alcohol. Smoking
- Medications that alter vascular tone or water-salt balance
- Chronic inflammatory lesions of the ENT organs: middle ear, nasopharynx
Important: the presence of risk factors does not in itself confirm Ménière's disease – they are merely guidelines for more accurate diagnosis and more effective preventative treatment and regimen recommendations.
Ménière's disease isn't uncommon, but it's not exactly a rare or exotic occurrence: ENT doctors and neurologists regularly see such cases. The condition can first manifest in adulthood, and people often attribute the symptoms to fatigue or vascular problems for a long time, until an attack becomes so severe that a doctor and a full diagnosis are required.
Ménière's syndrome and Ménière's disease are not the same. A syndrome is a similar clinical picture with a different cause: inflammation or injury, or a different pathology of the inner ear or central structures.
At the beginning of the examination, the goal is the same. The diagnosis must be verified. Confirm Ménière's disease, not just a description of the symptoms.
Classification and stages

Stages of Meniere's disease
The course of Ménière's disease is described in stages. The criteria are simple: the severity of attacks and hearing dynamics. In the initial period, attacks of vertigo are difficult to tolerate. After an episode, hearing may partially recover, with significant fluctuations possible. Subsequently, the hearing loss becomes more persistent. Tinnitus is persistent. The frequency of attacks may decrease, but hearing loss is impaired due to asthenia and increasing fatigue. With prolonged progression, the disease progresses to significant hearing loss on the affected side. At this stage, the goal of treatment shifts to symptom control, maintaining quality of life, and preventing falls.
To make it clearer, here's how it typically looks in practice:
- Early stage. Attacks of vertigo. Hearing fluctuations. Tinnitus occurs episodically.
- Advanced stage. Episodes occur more frequently. Hearing loss becomes noticeable. Recovery after an attack is incomplete.
- Late stage. Hearing loss is persistent. Severe attacks of dizziness may become less frequent and be replaced by constant unsteadiness and instability.
After this assessment, the doctor discusses the management strategy with the patient. Which treatment methods are appropriate at the current stage? What preventive measures are needed now? And what may be needed as the disease progresses.

Types of Meniere's disease
In clinical practice, variants of Ménière's disease are distinguished based on the underlying syndrome. This is determined by which system is primarily affected—the auditory or vestibular system.
With the vestibular variant, attacks of vertigo and severe instability are prominent. With the cochlear variant, hearing loss and persistent tinnitus predominate. This approach helps explain the differences in the clinical picture between patients and more accurately determine treatment strategies.
- Vestibular variant: marked balance disturbances predominate, with a sensation of rotation, instability, and nausea; Hearing function may change unevenly.
- Cochlear (auditory) variant: noise, ear fullness, and hearing loss are prominent, while dizziness is less pronounced or occurs less frequently.
- Mixed variant: both vestibular symptoms and hearing loss are significant; the course may progress, with alternating periods of relative improvement and exacerbations.
Sometimes Ménière's syndrome begins as a cochlear variant. Initially, noise and hearing loss predominate. Typical vestibular attacks then develop. Therefore, the diagnosis is clarified dynamically. Examination and observation help determine the form of the process. Then, treatment options can be selected.

Clinical picture
Symptoms
In Ménière's disease (and the variant known as Ménière's syndrome), two functions of the inner ear are involved: hearing and balance. Therefore, the condition changes abruptly. One moment everything is stable. The next – a severe attack.
For the doctor, details are decisive. Which symptoms occur together? How long does the episode last? What is the frequency and recurrence? The clinical picture guides the diagnosis and determines the treatment strategy.
- A sharp sensation of spinning of the surrounding space or being pulled to the side, making it difficult to stand and walk; Symptoms often worsen with head movements.
- Constant or increasing noise (ringing/humming) in one ear and a feeling of fullness, as if the "pressure inside" has increased.
- Floating hearing loss, when hearing may partially return after an attack, but as it progresses over time, a more persistent loss develops.
- Nausea, vomiting, and severe weakness during an attack; Sometimes cold sweat and tremors are added.
- Increased sensitivity to light and sounds, a feeling that any stimulus "overloads" the nervous system.
- Residual unsteadiness after an attack: vestibular discomfort does not immediately resolve, and instability persists for some time.
If attacks recur and are accompanied by noise, ear fullness, and hearing changes, consult a doctor immediately. Early diagnosis and treatment reduce the frequency of episodes, improve symptom control, and reduce the risk of falls and injuries.
Progress of the disease
The course of the disease can be unpredictable: in some people, the intervals between attacks are long, while in others, attacks occur in series. Often, warning signs appear before an episode—increasing noise, hearing changes, or a feeling of pressure in the ear. After an episode, weakness and instability may persist, which is important to consider in everyday life and at work. Even with the same name, "Ménière's disease," the symptoms vary from person to person—so advice like "what someone told you" is the least helpful, and a personalized diagnosis and treatment plan are the most helpful.
Diagnosis of Meniere's disease
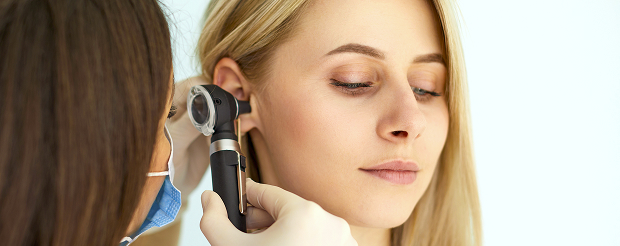
The examination is comprehensive. The doctor compares the patient's subjective complaints, the physical examination, and the information obtained during functional testing. The main goal of this approach is to confirm that the source of the problem is in the inner ear, as well as to consistently rule out other possible causes of dizziness, including nervous system disorders, vascular disorders, and medication effects.

Diagnostic methods
The doctor typically begins with a detailed interview: how long the attack lasts, what triggers it, how hearing changes, whether there is noise, and whether there have been episodes of otitis media. An ENT examination and neurological assessment are then performed to determine which part of the vestibular system is involved and the likelihood of Ménière's disease or syndrome.
- Detailed collection of complaints and anamnesis (frequency, duration, triggers, nature of dizziness, hearing changes, sensation of pressure)
- ENT examination with assessment of ear condition and possible middle ear problems
- Neurological assessment to rule out other causes and clarify vestibular disorders
- Symptom history: attack diary (time, duration, trigger, severity of nausea, hearing changes, and noise)
Before instrumental examinations, it is useful to collect this data in advance: this simple method makes diagnosis more accurate and helps the doctor quickly select the optimal treatment and further examination plan.
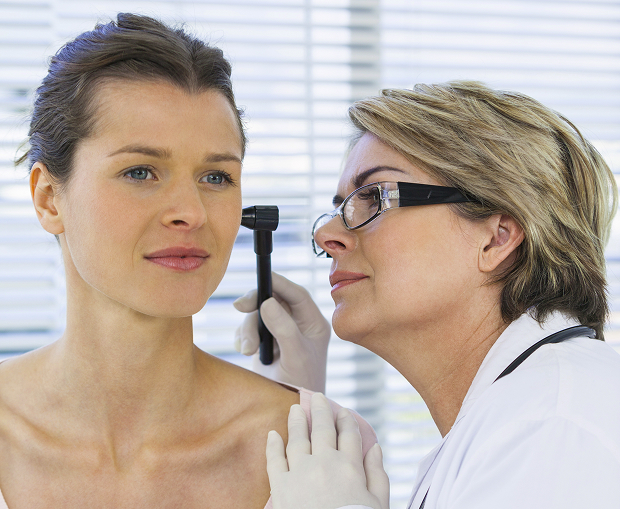
Diagnostic criteria
In clinical practice, the diagnosis is based on a combination of recurring episodes of rotational vertigo and documented hearing changes, as well as the presence of noise/fullness in the ear.
A single attack is not enough for diagnosis. Recurrence is required. A characteristic symptom trend is needed (how hearing, noise, and a feeling of pressure in the ear behave before, during, and after the episode). If the picture is still incomplete, the doctor diagnoses "probable Ménière's syndrome." The doctor then continues to monitor the patient's condition.
Instrumental diagnostics
Instrumental examination methods provide an objective examination of the auditory system. They also test the mechanisms responsible for balance. Specific hearing tests are typically used, such as stability and coordination tests. In some cases, imaging techniques are used to rule out concomitant or alternative causes of the symptoms. The scope of diagnostics is determined on an individual basis. Some patients present at the onset of the disease. Some are already at the stage of noticeable hearing loss, as well as regular episodes.

Laboratory tests
Laboratory tests do not directly "prove" the disease. However, they do provide an opportunity to identify underlying systemic factors. These may include inflammation, metabolic disorders, or signs of autoimmune processes. If a secondary syndrome is suspected, laboratory diagnostics are especially useful. This is necessary to avoid missing a cause that can be treated specifically.
Methods of treatment for Meniere's disease
Treatment for Méniere's syndrome involves stopping an acute attack, as well as long-term conservative therapy and lifestyle modifications. In some cases, surgical treatment is the only option. The goal is to reduce the frequency and severity of attacks, stabilize hearing, and reduce the risk of falls. It's important to note that treatment is a process: the plan may change as the disease progresses or, conversely, "calms down."
Treatment of an acute attack
During an attack, safety and symptom relief are paramount. Doctors recommend rest, a dark, quiet room, and minimal head movements. Medications are prescribed to reduce nausea and suppress severe vestibular discomfort. These medications also affect fluid circulation and blood pressure (as indicated). Severe episodes accompanied by dehydration due to vomiting are treated in a day hospital setting. 24-hour observation may also be necessary.
Important note: self-medication is dangerous because Ménière's syndrome can sometimes mask other conditions.
- If the first severe attack with neurological symptoms (numbness, weakness, speech impairment) occurs, acute vascular causes should be immediately ruled out.
- If dizziness is accompanied by a high fever and pain, inflammation should be assessed.
- If sudden hearing loss occurs, act quickly to avoid wasting time.
After this, the doctor returns to the plan: what to do next to reduce the frequency of recurrences.
Conservative treatment
Conservative therapy includes a regimen, diet, and medication. The basic approach is aimed at stabilizing fluid and salt balance. Salt intake is limited, sleep is normalized, and stress is reduced. This maintains fluid balance in the inner ear and reduces the likelihood of triggering an attack.
Drug therapy is selected based on the underlying syndrome. In some cases, the priority is to control vertigo attacks quickly and according to a specific plan. In others, noise reduction and stabilization of hearing function are key. However, progress is assessed throughout the course of treatment. If compensation is insufficient, vestibular rehabilitation is initiated. A set of exercises is aimed at developing central compensation and improving postural control.
Surgical treatment
If conservative treatments are ineffective, interventions targeting the endolymphatic system (e.g., the endolymphatic sac) or the structures responsible for seizures are considered. The decision is made after repeated diagnostics and risk assessment, as the priority is to preserve hearing and quality of life.
Before choosing a treatment strategy, the doctor will compare the frequency of seizures, hearing dynamics, and the severity of the patient's vestibular impairment.
Preventive treatment
Prevention is a systematic plan. It includes risk factor monitoring, specialist observation, and therapy adjustments. It also includes teaching the patient how to recognize attack warning signs. This reduces the risk of injury and significantly increases confidence in everyday life.
Why is it better to treat Meniere's disease at K+31 clinics?
When choosing a clinic for treatment, it's not just the "closest" location that matters, but also how convenient the entire process is: from the initial consultation to follow-up visits. At K+31 clinics, this is easier thanks to clear navigation by specialty, the ability to book online, select a specialist, and comprehensive diagnostics all in one place. A plus is the availability of inpatient care and observation if an attack is severe or requires intensive care. It's also convenient to quickly move from an ENT specialist to related specialists and examinations, without wasting time on separate visits.

FAQ
Is it possible to completely cure Ménière's disease?
How common is Ménière's disease?

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Price
Other services






































































Ménière's disease progresses in waves. A period of rest can be interrupted at any moment by a sudden attack. After an attack, the patient experiences:
The main danger: during and after an attack, motor coordination is impaired. In this state, driving, crossing the road, and performing household chores that require precision are dangerous. Work performance declines during this period.