Tympanometry

specialists
equipment
treatment

When is tympanometry prescribed?
- Difficulty hearing sounds when the cause is unclear, especially in children
- Hearing loss after an illness
- Hearing problems resulting from a head injury
- Recurring ear infections
- Recurring colds or sinus infections. Infections easily spread from the nasopharynx to the ear through the eustachian tube, causing otitis media.
- Suspected polyps or other growths in the ear.
- Adenoid inflammation.
- This method is often used in addition to audiometry to clarify the diagnosis, as it alone cannot determine the degree of hearing loss.
Purpose and essence of the study
The goal of tympanometry is to quickly and objectively assess the condition of the middle ear and the mobility of the system responsible for sound conduction. During the examination, the device creates controlled pressure in the ear canal and records the eardrum's response to the sound signal, so the doctor obtains data not through verbal feedback but through measurements. Additionally, the ventilation through the eustachian tube and the freedom of vibration transmission through the auditory ossicles are assessed—this is important for understanding where sound conduction is impaired.
This method helps identify disturbances in the sound conduction mechanism and suspect pathologies that are often hidden during a routine examination: fluid in the middle ear, eustachian tube dysfunction, eardrum perforation, as well as conditions in which the eardrum becomes excessively rigid or, conversely, excessively mobile. Tympanometry doesn't measure "how much a person can hear" in loudness figures, so it's usually supplemented by audiometry. Together, these methods enhance diagnostics and help more accurately determine further treatment.

How is tympanometry performed?
The test is quick and generally painless: the procedure is felt as gentle pressure or a popping sensation in the ear for a few seconds. During the measurement, it's important to sit still and maintain a steady head position to ensure the probe maintains a seal in the external auditory canal. It's also best not to speak, swallow, or chew, as any movement can affect the eardrum's response and the accuracy of the results.
The probe emits a beep and changes pressure, and the device records the middle ear's auditory response. The result is a tympanogram—a graph that shows the eardrum's mobility and sound conduction characteristics. The doctor analyzes the tympanogram along with your complaints and physical examination, then explains the meaning of the results and whether further testing (such as a hearing analysis with audiometry) is needed.

Indications for tympanometry
Tympanometry is performed when indicated to evaluate middle ear function and determine the cause of hearing loss; a doctor will refer you for the test.
- Difficulty perceiving sounds, especially in children, when the cause is unclear
- Hearing loss after an illness
- Hearing problems after a head injury
- Recurring ear infections (otitis)
- Frequent colds/sinus infections affecting the eustachian tube
- Suspected ear tumors
- Adenoid inflammation
This method is often supplemented with audiometry: together, the tests more accurately explain the cause of hearing loss and the appropriate treatment.

Contraindications to tympanometry
Tympanometry has contraindications, and situations in which the procedure is temporarily postponed to avoid increasing pain and distorting the results. This primarily applies to acute inflammation of the ear with severe pain, when any impact on the external auditory canal causes discomfort. The test is also not performed in cases of bleeding, recent trauma, suspected foreign body, or severe swelling that prevents hermetic placement of the probe. A separate, important consideration is the possibility of a breach: if a ruptured eardrum is suspected, the doctor first assesses the condition during an examination and determines the safest approach.
- Acute inflammation with severe pain
- Bleeding or recent ear injury
- Suspected foreign body
- Severe swelling/inflammation of the external auditory canal
- Suspected eardrum damage (pending further investigation)
The final decision on whether the examination can be performed is made by the physician after the examination.

Preparing for the study
No special preparation is usually necessary: you don't need to arrive on an empty stomach, and the test itself takes just a few minutes. It's important to ensure the probe fits snugly and accurate measurements are obtained. Avoid deep cleaning with cotton swabs before the appointment, as this can injure the skin of the external auditory canal or push wax deeper. If you have a fever, severe pain, a recent ear injury, or discharge, it's best to inform the doctor in advance; the procedure may be rescheduled or modified.
Before the procedure, the doctor usually performs an otoscopy: they examine the ear canal and eardrum, ruling out inflammation and obstructions to the measurement. If wax or significant contamination is detected, cleaning is addressed first; otherwise, the test may be inaccurate. Bring your previous examination results (if any) with you; this will help the doctor compare the progress and interpret the results more quickly.
Diagnostic results and their interpretation
The result of tympanometry is a tympanogram: a graph that shows how the middle ear system's response changes with controlled changes in pressure in the ear canal. Essentially, it's a "map" of the degree of mobility of the eardrum and associated structures in a given patient's condition. Proper interpretation always takes into account the patient's complaints and examination data, so the same graph can be interpreted differently in different clinical situations. Below are the main types of tympanograms and their diagnostic significance.
Interpretation of tympanometry results
Tympanometry presents results as diagrams, where the primary markers are the peaks. The presence or absence of these peaks, their number, and their size allow us to assess the health of the middle ear. There are six basic diagram types:
1. Type A: A single central peak symbolizes normal ear function. This means that the eardrum and ossicles are functioning properly, and the pressure in the eardrum is normal.
2 Type B: No peaks on the graph may indicate problems, including scarring of the eardrum, fluid in the ear, or tumors.
3 Type C: A peak located in a low-pressure zone may indicate partial or complete blockage of the Eustachian tube.
4 Type D: The presence of two peaks is a sign of excessive mobility of the eardrum, possibly due to its thinning or damage.
5 Type E: Multiple peaks or a single peak with a split peak may indicate a problem in the sound transmission system, possibly due to damage to the ossicles or inflammation.
6 Type Ad: An excessively high peak, extending beyond the normal range, indicates increased mobility of the eardrum when probing at low frequencies.
General information about the procedure
Tympanometry prices in Moscow
The price of tympanometry in Moscow is determined by several factors, so the final cost may vary even for identical complaints. First, the scope of the test affects the procedure: one ear or both ears are tested, which changes the duration of the procedure and the amount of data collected. Second, whether a separate consultation with an ENT specialist is required before/after the test and whether an extended report explaining the results is required is considered. Third, the cost is affected by the diagnostic program: tympanometry is often supplemented by audiometry and other tests to more accurately assess hearing and the cause of the hearing loss. Urgency (for example, an appointment "for today") and the need for follow-up monitoring may also be considered.
The price is usually calculated in rubles, and it's more convenient to confirm the exact cost at the clinic: by phone, through the appointment form, or in the price list on the website. This way, you will understand in advance what the service includes and which options are truly necessary for your specific case.


This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Price


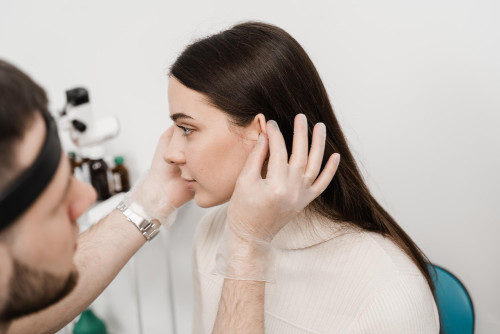
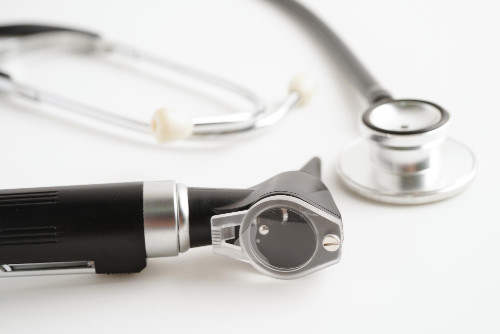




























































What is tympanometry?
Tympanometry is an objective testing method used to diagnose middle ear diseases. During the test, the device gently changes the pressure in the external auditory canal and delivers a sound stimulus, then records the response of the eardrum and middle ear system. Using a tympanogram, the doctor evaluates the mobility of the eardrum, the function of the eustachian tube, and signs of fluid or inflammation that may reduce hearing comfort. Tympanometry is often supplemented by audiometry to obtain a more complete picture of hearing and determine further treatment.