Sinusitis treatment

specialists
equipment
treatment
Types
Depending on the cause and course of the disease, sinusitis can be divided into the following types.
Infectious (viral, bacterial, fungal) sinusitis
When the immune system is compromised, bacteria or infections enter the body through the blood or respiratory tract. Inflammation is caused by Haemophilus influenzae, chlamydia, staphylococcus, streptococcus, and various types of fungi. This type of sinusitis most quickly progresses from the normal form to purulent. Is this type of sinusitis contagious? Only through direct and close contact with an infected person.
Allergic sinusitis
The main cause is allergic rhinitis, which most often occurs in the spring or fall. This type of sinusitis causes nasal swelling and irritation of the mucous membrane. The condition is paroxysmal, characterized by constant nasal congestion, persistent sneezing and discharge, and itching.
Vasomotor sinusitis
This unusual name conceals a nasal breathing disorder caused by a narrowing of the nasal passage. The main cause of the vasomotor type is a change in the excitability of the autonomic nervous system, resulting in an inadequate response to external physical stimuli.
Vasomotor sinusitis is further divided into two types:
- Allergic
- Neurovegetative, i.e., caused either by endocrine disorders or abnormalities of the nasal septum, as well as by prolonged use of vasoconstrictors (xylometazoline, naphazoline, etc.)
Both of these types are characterized by breathing and sleep disturbances, poor appetite, weakness, headaches, and fatigue.
Exudative sinusitis
The name comes from the word "exudate," a fluid that accumulates in the sinus during acute inflammation. In this form, serous and purulent discharge emerges from the nose. This discharge lingers in the nose, dries, and crusts over. In more severe cases, the exudate is more watery, and the mucus comes out in patches, draining into the nasal cavity when the head is positioned in certain positions.
Productive sinusitis
This type is subdivided into:
- Caseous
- Mural hyperplastic
- Atrophic
- Polypoid
- Necrotic
- Cholesteatoma
During productive sinusitis, polyps form, and the mucous membrane inside the sinus grows and becomes deformed. When the mucous membrane thickens, fluid does not form within it.
Necrotic sinusitis
This type of sinusitis is the most complicated stage. It causes necrosis, or tissue death, in the sinus. It cannot be cured with medication alone; surgical intervention is required. When the posterior sinus wall dies, an extradural abscess, meningitis, and even a brain abscess develop.
Atrophic sinusitis
This form is accompanied by atrophy (i.e., partial death) of the mucous membrane. With atrophic sinusitis, nasal discharge has an unpleasant odor, and the patient may experience sinus pain.

Reasons
The disease can be caused by various factors:
- The main cause is colds and acute respiratory infections, as they are accompanied by a runny nose, and tissue swelling and mucus accumulation create a favorable environment for the growth of bacteria and fungi.
- Hypothermia and constant exposure to cold air and drafts also lead to colds and runny noses, which can lead to sinusitis and exacerbation of the chronic form of the disease.
- Allergic reactions
- Congenital anomalies: deviated septum, etc.
- Trauma to the nasal septum and surrounding bones and cartilage
- Infections, bacteria, or fungi
- Adenoids and polyps forming in the nasal cavity
- Serious illnesses such as tuberculosis, radiation sickness, fungal infections, etc.
It's important to remember: many of these causes are interconnected, and all of them lead to tragic consequences if a person self-treats or delays treatment altogether.

Pathogenesis of sinusitis
Sinusitis develops as a sequential chain of changes in the mucous membrane: first, inflammation and swelling occur in the area of the ostium, through which the sinus communicates with the nasal cavity. Due to the narrowing of this "exit," ventilation and drainage of secretions from the maxillary sinus are impaired, causing exudate to accumulate within. This congestion creates favorable conditions for the proliferation of microorganisms: infection sets in, the inflammatory response intensifies, blood pressure rises, and characteristic symptoms appear. This is how the disease develops, which without adequate treatment can prolong or become more prolonged.
Symptoms of sinusitis
The disease can be distinguished by several signs:
- Nasal congestion and discharge. As a result of swelling of the mucous membrane and stagnation of fluid, a person is tormented by a feeling of pressure in the sinuses
- As the disease worsens, severe and prolonged headaches begin. Pain in the bridge of the nose and temples also appears
- The temperature rises to 37-38 degrees
- Weakness, memory and concentration may deteriorate
- Decreased performance and rapid fatigue
Please note that not all of these symptoms necessarily appear together - the disease may be accompanied by only a couple of these signs.
Symptoms of sinusitis in adults
Sinusitis is equally unpleasant for people of any age, regardless of gender. In adults, the disease is characterized by:
- Pain in the nose that increases over time. Usually, it's almost absent in the morning, but intensifies towards evening. Sometimes, the pain extends from a specific area to the entire head.
- The nose becomes stuffy, and the voice becomes nasal.
- Clear or greenish (purulent) nasal discharge is observed.
- If the nose is very stuffy, sinusitis without a runny nose, i.e., without discharge, is possible.
- In the acute stage of the disease, the temperature reaches 38 degrees Celsius, and sometimes even higher. But if sinusitis becomes chronic, there are no temperature fluctuations.
- Sleep disturbances
- Decreased appetite
- Tonsillitis or pharyngitis may develop, resulting in a sore throat and cough.
In more advanced cases, loss of smell, tearing, sweating, bad breath and nose, and a strange taste in food may also occur.
Symptoms of sinusitis in children
Sinusitis is generally uncommon in young children under 3-4 years old, as their sinuses are not yet fully developed. A little later, it can occur with a runny nose and resolve easily. However, its symptoms should not be ignored:
- High body temperature
- Poor sense of smell, i.e., inability to distinguish odors
- Pain in the maxillary sinuses, especially when bending down
- Nasal congestion
If you observe any of these symptoms in your child, it is worth taking them to a doctor to prescribe the correct and timely treatment.
Symptoms of acute sinusitis
Acute sinusitis usually begins rapidly: severe nasal congestion, pressure, and a feeling of fullness in the cheeks, which intensifies when tilting the head. A common symptom is pain in the maxillary sinuses, sometimes radiating to the upper teeth, forehead, or temples. Fever, weakness, and a decreased sense of smell are common, as well as thicker, discolored nasal discharge.
Symptoms of chronic sinusitis
Chronic sinusitis often presents with a vague and prolonged course: nasal congestion may be constant or intermittent, with periods of improvement and worsening. A typical symptom is a dull, moderate ache or heaviness in the face, especially in the evening, with a temperature often normal or low-grade. Persistent discharge, mucus dripping down the back of the throat, a nighttime cough, decreased sense of smell, and fatigue are common, with exacerbations occurring as acute episodes.
Diagnosis of sinusitis
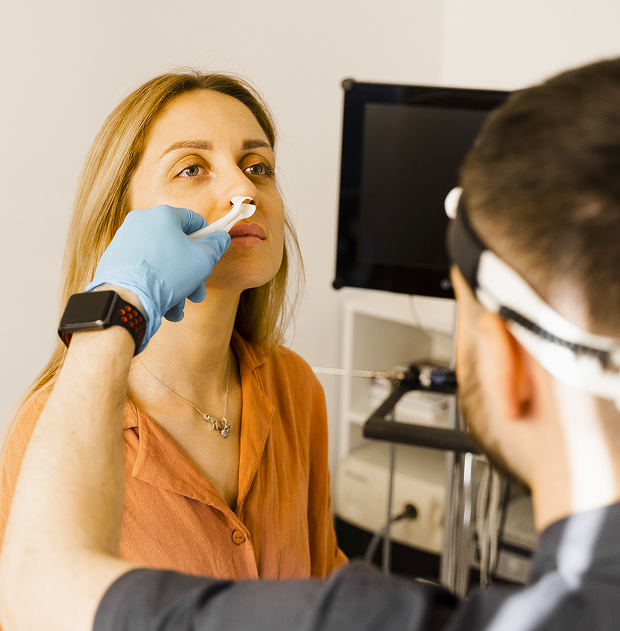
Collecting anamnesis
The first stage of diagnosis is a consultation: the doctor asks how long the complaints have been present, what was present initially (a cold, allergies), whether there is a "second wave" of worsening symptoms, and how the discharge has changed. It is important to understand the patient's observations: the location of the pain, its association with tilting the head, decreased sense of smell, episodes of fever, and the effect of treatment. This data collection helps suspect a bacterial infection and determine the appropriate diagnostic method.
Laboratory Diagnostics
Laboratory tests are not always necessary, but they strengthen the clinical judgment in severe cases or in doubt. Signs of an inflammatory reaction are most often assessed in blood tests to indirectly confirm the activity of the process and the likelihood of a bacterial infection. In cases of prolonged or frequent relapses, the doctor may prescribe additional tests to clarify the underlying cause and reduce the risk of inappropriate treatment.
Instrumental Diagnostics
Instrumental diagnostics help confirm sinus involvement and assess the extent of the process. The primary approach is an ENT examination (including endoscopy if indicated), and imaging is selected based on the specific case: CT is more informative for the sinuses, MRI is used in certain situations, and X-rays are used sparingly. The doctor selects the method based on symptoms, the risk of complications, and the patient's current condition.
Methods for treating sinusitis
The treatment depends on the cause and severity: with a viral infection, observation and local measures are often sufficient, while signs of bacterial inflammation require a more aggressive approach. A conservative approach is the standard, especially if this is a first episode and there are no complications. Treatment is selected separately for adults and children, taking into account age, comorbidities, and tolerance. The goal is to restore sinus drainage, reduce swelling, control the infection, and prevent progression to chronicity.
Conservative treatment
Conservative treatment aims to alleviate symptoms and restore normal sinus drainage without intervention. A regimen, adequate fluid intake, humidification, and irrigation are typically recommended to help the mucus become less viscous and drain better. In children, it's important not to overdry the mucus and strictly adhere to the prescribed dosage. In adults, the risks of self-medication with decongestants should be considered.
Drug therapy
Medications are prescribed based on the clinical picture: one drug reduces swelling and improves ventilation, another reduces inflammation and pain, and a third affects the viscosity of mucus. Antibiotics are not always necessary: they are used when a bacterial infection is likely (for example, a protracted course without improvement, a "second wave" of deterioration, or a severe onset), and the doctor decides the regimen. Additionally, allergy medications may be used if the underlying condition is appropriate, as well as medications to control fever and discomfort.
Hardware methods
A hardware-based method is chosen when it's important to quickly restore patency and improve nasal drainage. These options include vacuum irrigation ("cuckoo") and a sinus catheter, which help evacuate contents and deliver solutions locally. These procedures can be an effective complement to medication if performed according to indications and in the correct regimen, rather than as a "just in case" course.
Invasive treatment methods
Invasive methods are necessary if conservative treatment fails, significant accumulation of contents persists in the sinus, or there is a risk of complications. The main goal is to quickly restore drainage and sanitize the sinus, allowing for more stable treatment.
Maxillary sinus puncture
Puncture relieves pressure, evacuates contents, and rinses the sinus; if necessary, samples are taken for analysis. The procedure is performed under local anesthesia, and the indications are determined by an ENT specialist after an examination and testing. Drug therapy is then usually continued to control the infection and restore the mucosa.
Endoscopic antrotomy
Endoscopic antrotomy is used when an outflow obstruction needs to be removed: to widen the ostium, remove polyps, or resolve the anatomical cause of a chronic condition. The procedure is performed through the nose without external incisions and is controlled by an endoscope. After surgery, medical monitoring and proper care are important to reduce the risk of recurrence.
K+31 photo gallery

Our doctors
Make an appointment at a convenient time on the nearest date

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Price
Other services

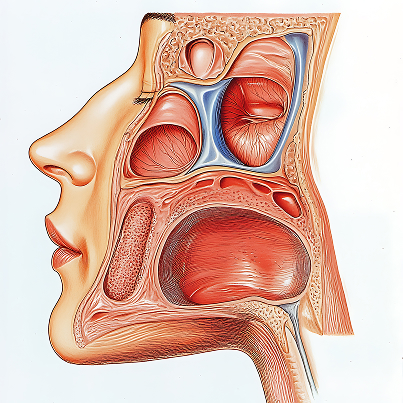

































































Definition of sinusitis
Sinusitis is an ENT disorder characterized by inflammation in the maxillary sinus, either on one side or both. This paranasal cavity communicates with the nose through narrow openings, so any significant swelling of the mucous membrane quickly disrupts ventilation and the natural drainage of secretions. When drainage is blocked, conditions arise for the accumulation of secretions, increasing pressure, and the development of characteristic complaints, ranging from congestion to pain in the cheeks and upper teeth. Medically, this process is a process in the paranasal sinuses, which can be associated with a viral infection, bacteria, allergies, or dental problems.