Impetigo in children
Impetigo in children is a superficial skin infection characterized by the appearance of a blister, erosions, and characteristic crusting. The disease is contagious, so it often spreads quickly within a family or group of children, especially if the child has close contact with other children.

specialists

equipment

treatment

Causes of impetigo
The disease develops when bacteria enter damaged skin. Most often, these bacteria are staphylococcal or streptococcal. Mixed infections are also common. Bacteria quickly establish themselves on the skin if it is irritated, scratched, or constantly wet.
Predisposing factors
There are situations in which the disease occurs more frequently. These occur when the integrity of the skin is compromised. Below we list typical factors, but it is important to remember that a doctor evaluates the progression of the disease individually for each age and case. Causes of the disease:
- Microtrauma, scratching from insect bites, atopic itching
- Skin maceration due to sweating and frequent contact with water
- Runny nose and runny nose in children (irritation around the nose and mouth)
- Close contact in a group, shared towels, toys
- Decreased immune defense after viral infections
Once the factors are identified, it is easier to develop preventative measures and reduce the likelihood of recurrence, even if treatment is successful.
Pathogenesis
The bacteria enter the upper layers of the epidermis through damage. They then begin to multiply, triggering an inflammatory process. A blister containing cloudy fluid then forms, which then bursts, leaving the skin wet and eventually forming a crust. At this stage, the disease is contagious. If staphylococcus aureus (staph) is present, larger bullous lesions develop. If the child scratches the skin vigorously, the infection quickly spreads throughout the body.
Symptoms of impetigo
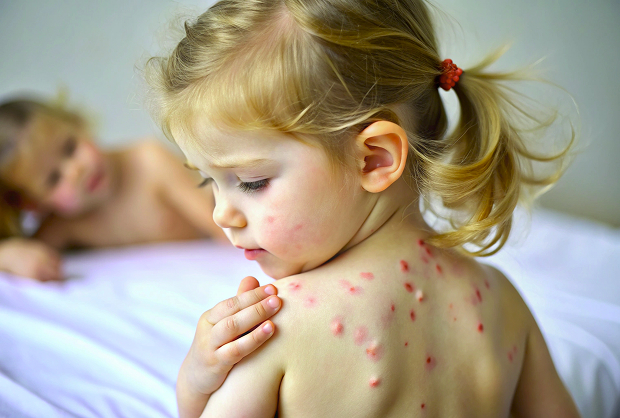
Manifestations by external signs
The external characteristics of the disease are blisters that burst, ooze, and then form crusts. The location of the blisters depends entirely on the location of the initial epidermal damage, where the child transmits the infection.
The main signs of the disease include small superficial blisters that burst within 24 hours, oozing erosions followed by the formation of yellowish-honey crusts, redness and irritation around the lesion, and moderate itching. Affected areas include the face, hands, and the area around the mouth and nose. The appearance of the blisters alone cannot immediately determine whether the disease is caused by streptococcus or staphylococcus. Therefore, to accurately determine the form of the disease, the doctor relies on a dynamic examination and, if necessary, prescribes diagnostic tests.

Manifestations by occurrence
Impetigo can present differently. In one child, the disease begins in a single area, while in another, it can develop in several areas of the body at once, meaning multiple lesions are observed, especially if the epidermis is scratched. The rate of spread is not related to the severity of the disease; it is directly related to the habit of touching the scratched areas and spreading the infection to adjacent areas of the body.
So, the disease begins with a single lesion after a microtrauma, such as a bite or skin irritation. New lesions then quickly appear, especially if the child frequently scratches the skin. Gradually, the lesions spread across the face and hands. A wave-like progression, where old crusts dry up but new blisters appear nearby, also contributes to the spread of the disease. If the number of lesions increases, signs of a bullous form, meaning large blisters, appear within 1-2 days. Therefore, it's best not to delay a visit to the doctor; it's essential to see a specialist as soon as possible, as early impetigo treatment in children can significantly reduce the time it takes to treat.
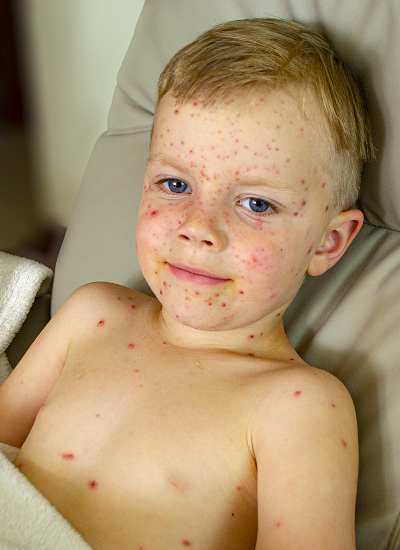
Classification and stages of impetigo
Classification is necessary to choose a strategy: topical treatment, systemic antibiotics, or a combination approach. The doctor also clarifies whether the process is primary (on healthy skin) or secondary (due to dermatitis, scratching, or chronic lesions).
Before listing, it is important to note that the forms can progress from one to another if the child actively injures the skin or the infection spreads.
- Non-bullous form (often streptococcal impetigo in children): small blisters that burst quickly and form honey-colored crusts.
- Bullous form (bullous impetigo in children): larger, flaccid blisters, often associated with staphylococcal toxins.
- Mixed form: signs of both streptococcal and staphylococcal infection.
- Ecthyma (rare): deeper skin lesion, takes longer to heal, and requires careful treatment.
The stages are usually: blister appearance → bursting/oozing → crust formation → healing. If there is active contact with others during the oozing stage, the infection spreads especially quickly.

Complications of impetigo
Complications arise when treatment is started late, the lesions are large, or the child constantly scratches the skin. Sometimes new bacteria are introduced, and the process becomes more protracted.
- Spread to new areas of skin, multiple lesions
- Painful cracks, secondary inflammation, lymphangitis
- Worsening of underlying dermatoses
- Scars with deeper lesions and prolonged inflammation
To reduce the risk of complications, it is important not to pick at scabs or cauterize them with harsh solutions without a doctor's prescription.
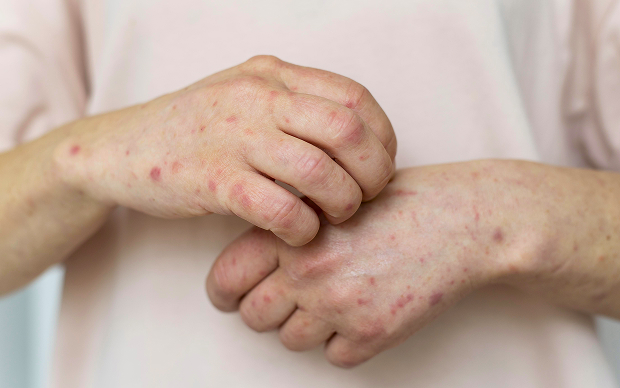
Risk groups for developing impetigo
There are children who are more likely to develop impetigo due to their skin condition, social environment, and caregiving practices. The risk is higher in preschool age, when contact is close and hygiene practices are still imperfect.
- A child with atopic dermatitis, eczema, or frequent itching
- Children attending preschool/kindergarten where equipment is shared and there is close contact.
- Chronic infection foci (e.g., frequent rhinitis with skin irritation)
- Hot weather, sweating, skin maceration
If a child is at risk, prevention and early diagnosis are especially important to prevent the disease from recurring.

Diagnosis of impetigo
Diagnosis is usually clinical: an experienced physician can quickly suspect impetigo based on the appearance of the rash and its dynamics. However, if the course of the disease is atypical, there are frequent relapses, or a suspected mixed infection, further testing may be necessary to more accurately select a treatment and avoid blindly prescribing an antibiotic.
Before the list, an important thought: the goal of the examination is not to "test everything," but to determine the form and pathogen if this affects the treatment plan.
- Skin examination to assess the location, type of lesions, and extent of the lesion.
- History taking: when the rash appeared, whether there was fever, itching, or contact with sick people.
- If necessary, a bacterial culture/smear from the lesion to determine the staph or streptococcal pathogen and sensitivity.
- Assessment of underlying skin problems (atopy, scratching) that contribute to the disease.
After the examination, the doctor explains to the family how long impetigo treatment takes in children, when the child becomes no longer contagious, and how to care for the skin at home.
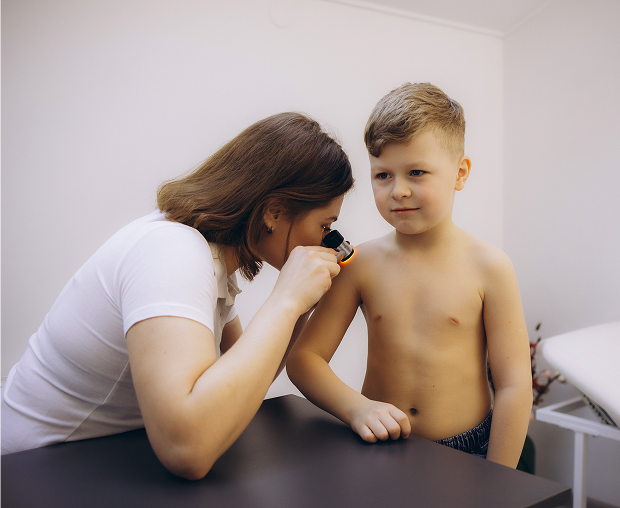
Differential diagnostics
This condition is often confused with herpes, allergic dermatitis, and even chickenpox. Impetigo also resembles contact infections and candidal lesions. Sometimes, a fungal abscess is mistaken for impetigo. When blisters appear on the skin, it's important to completely rule out rarer dermatological conditions.
To avoid making a mistake in diagnosis, the doctor relies on a combination of signs. The specialist observes the appearance of the blister and how quickly it bursts. They monitor the presence of typical crusts, the extent of the lesions' spread, and how the skin responds to treatment.
If in doubt, the specialist prescribes laboratory diagnostics. This reduces the risk of unnecessary or improper use of antibiotics and significantly speeds recovery. If a child's rashes recur, the doctor evaluates possible sources of reinfection in the family. The fact is that an adult carrier can maintain the circulation of bacteria, so reinfection occurs.
Treatment of impetigo
Treatment tactics depend entirely on the severity and extent of the disease. For small lesions, topical therapy is sufficient, but if a child has multiple skin lesions, a systemic antibiotic may be required. However, the primary goal of treatment is to quickly stop the infection, reduce contagiousness, and restore the skin barrier to prevent recurrence of impetigo.
Conservative treatment
This involves treating the lesions using medications that target the causative agent. The doctor selects medications based on the type of infection—streptococcal or staphylococcal—and the severity of the condition. Treatment includes topical antiseptics and antibacterial ointments, as prescribed by the doctor.
For a widespread abscess, a systemic antibiotic is mandatory, taking into account the clinical presentation of the condition. A culture is taken if necessary. Gentle skin care is also prescribed, which involves cleansing the epidermis without trauma. Underlying conditions are also treated. For example, itching in dermatitis is controlled to prevent the child from scratching the lesions and preventing the disease from spreading throughout the body.
After the course of treatment, the specialist will evaluate the results. If the crusts disappear, new blisters do not appear, and the skin heals, then the treatment was chosen correctly and has yielded a positive result—a full recovery.
Surgical treatment
In some cases, surgical treatment is recommended; however, it is rarely necessary and does not represent the standard of care. Surgical treatment is considered only in isolated clinical cases, and only when large, painful, purulent complications develop. In this case, the doctor performs incision and drainage. Surgical treatments are also used when large lesions require treatment under the doctor's supervision.
Even in this case, antibacterial therapy and skin care are essential. After the procedure, the doctor provides clear recommendations for dressings and hygiene. This is necessary to prevent reinfection of the affected area. It is also imperative to eliminate the source of recurrence. Avoid scratching the skin, treat the dermatitis, or eliminate any family history of the disease. Otherwise, the disease will recur.
Why is it better to treat impetigo in children at K+31 clinics?
If your child shows signs of a skin infection, it's important to see a doctor as soon as possible. A clear procedure and the ability to involve related specialists is crucial for prompt treatment and recovery.
Our clinic offers convenient consultations, diagnostics, and full treatment monitoring, all in one place, making it very convenient for parents. You can schedule an appointment online or by phone. It's important to start treatment promptly, which is especially important when impetigo often spreads within days.
Another advantage of treatment at our clinic is our systematic approach. The doctor assesses both the source of the infection and the underlying causes that can cause recurrence. The specialist also creates a treatment and prevention plan to help quickly cure your child and prevent further infection.

Our doctors

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Price
Other services

























































































What is impetigo?
Impetigo in children is a superficial skin infection characterized by the appearance of vesicles, erosions, and characteristic crusts. The disease is contagious, so it often spreads quickly within a family or group of children, especially if the child has close contact with other children. Impetigo is sometimes colloquially referred to as "streptoderma," although this is essentially a general term for skin lesions that can be caused by both streptococcal and staphylococcal bacteria.
The forms of the disease vary. The streptococcal form often produces thin blisters or so-called "honey-colored" crusts. Bullous impetigo in children manifests as large, flaccid bullous lesions. In any case, regardless of the form of the disease diagnosed in a child, treatment should be initiated as quickly as possible. The sooner the infection is stopped, the lower the risk of complications and the lower the risk of infecting others, including adult family members.