Pancreatic cancer
Pancreatic cancer is a malignant tumor formed from the altered cells of the organ that secretes substances necessary for the digestion process and regulation of metabolism.

specialists

equipment

treatment
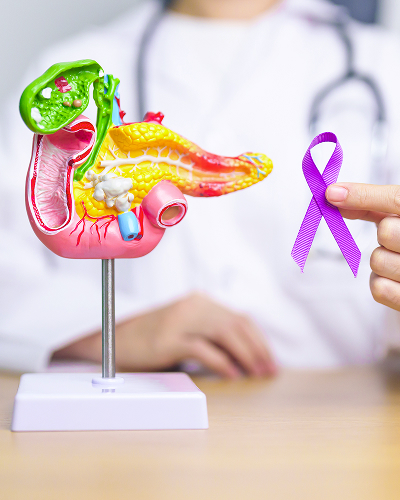
Prevalence of the Disease
Pancreatic cancer is one of the most pressing and complex problems in modern oncology. According to global statistics, this malignant neoplasm consistently ranks sixth in frequency of diagnosis among all oncological diseases. However, its true danger is revealed in its mortality rate – it accounts for approximately 7% of all cancer deaths, due to its extremely aggressive course and late detection.
The situation in Russia reflects global trends, demonstrating a steady increase in the number of new cases. This disease largely affects older patients, although its incidence has also been increasing in younger patients in recent years.
Regarding the localization of the pathological process, in more than half of all clinical cases, the tumor is detected in the head of the pancreas. In almost a third of patients, by the time of initial diagnosis, the disease has already reached widespread distribution, affecting the entire organ, which significantly limits radical treatment options and worsens the prognosis for each individual patient.
Experience an examination at the K+31 Clinic in Moscow to quickly detect diseases of the pancreas and other organs. We offer a full range of modern diagnostic procedures using expert-class equipment. We conduct a comprehensive analysis of all data during a consultation and provide accurate diagnoses in a short time.
Types of pancreatic cancer

Based on its secretory function, the pancreas is divided into exocrine and endocrine parts. The exocrine part secretes digestive enzymes, which are released through ducts into the duodenum. Endocrine tissue secretes hormones that go directly into the blood. Depending on which of these tissues the tumor formed in, exocrine malignant tumors of the pancreas are distinguished (the most common) and endocrine.
The most common endocrine tumor is adenocarcinoma. It can be ductal (formed in the glandular cells of the pancreatic ducts - the most common form of cancer) or acinar-cell (from the cells of the acinus - a special structure of the pancreas).
In addition to adenocarcinoma, pancreatic cancer varieties include such rare types as squamous cell carcinoma, undifferentiated cancer, cystadenocarcinoma, adenosquamous carcinoma, signet ring cell carcinoma.
Benign tumors can form in the pancreas, such as intraductal papillary tumor or cystic mucinous tumor. But they can degenerate into malignant tumors, so they are often removed surgically, especially if their location interferes with the function of the pancreas. Patients with such diagnoses should be examined regularly.
Endocrine cell tumors occur in less than 5% of cases. They are called neuroendocrine tumors, as well as islet cell tumors. According to the hormone secreted by the cells responsible for the formation of the tumor, neoplasms are called: gastrinoma (a tumor of cells producing gastrin), insulinoma (insulin), glucagonoma (glucagon), somatostatinoma (somatostatin). Usually these are benign tumors of the pancreas, but there are also malignant ones.
In rare cases, malignant tumors in the pancreas are metastases from cancer in another organ - this is metastatic cancer. The primary tumor can be in the gastrointestinal tract, kidneys, lungs, mammary gland or prostate gland. Sometimes the pancreas can be affected by metastases of melanoma (skin and mucous membrane cancer), osteosarcoma (bone cancer), leiomyosarcoma (smooth muscle cancer), Merkel cell carcinoma (skin cancer).
Location of pancreatic cancer
Cancer of the head of the pancreas
This is the most common type of pancreatic cancer by localization. Tumors in this part are smaller than in the body and tail, but due to the bile duct that passes here, even a small tumor can become a serious problem. It can compress the duct, which causes mechanical jaundice. A neoplasm in the head of the pancreas can also lead to a narrowing of the lumen (stenosis) of the duodenum. Another complication of malignant tumors of this localization is bleeding due to tumor decay.
Pancreatic body cancer
In terms of prevalence of pancreatic tumors, its body is in second place. Neoplasms here are larger than in the head. They can lead to inflammation of the vessels (thrombophlebitis), blockage of the lumen of the vessels (phlebothrombosis) and even diabetes. Advanced forms of pancreatic cancer localized in the body of this organ can cause jaundice.
Pancreatic tail cancer
This is the rarest type of pancreatic cancer in terms of location. But it is more difficult to diagnose using ultrasound.

According to the international TNM system, pancreatic cancer is divided into stages depending on the characteristics of three indicators:
- T – the degree of growth of the primary tumor: T1 – a tumor that has affected only the tissues of the pancreas up to its capsule, T2 and T3 – tumors at different stages of growth into the capsule and surrounding tissues and organs.
- N – the number of affected lymph nodes: N0 – the lymph nodes are not affected by the tumor process, N1, N2 and N3 – cancer has affected a different (increasing) number of lymph nodes.
- M – the presence of distant metastases: M0 – there are none, M1 – there are.
According to these indicators and their values, four stages of pancreatic cancer can be distinguished:
- Stage 1 – T1N0M0;
- Stage 2 – T1N1M0;
- Stage 3 – T1N2M0, T2N0M0, T2N1M0;
- Stage 4 – any values of T or N, but necessarily M1.

All cancers are caused by mutations in cells. There are many risk factors that can trigger such mutations. The most common risk factors for pancreatic cancer are:
- Type 2 diabetes
- Chronic pancreatitis – various inflammatory processes in the pancreas
- Gallstone disease
- Liver cirrhosis
- Cysts or adenomas in the prostate gland
- Smoking and alcohol consumption
- Predominance of fatty and spicy foods in the diet
- Burdened heredity
- Excess weight, especially excess fat in the waist area
- Age – the risk increases after 45 years, and most often the disease occurs at the age of 70 years
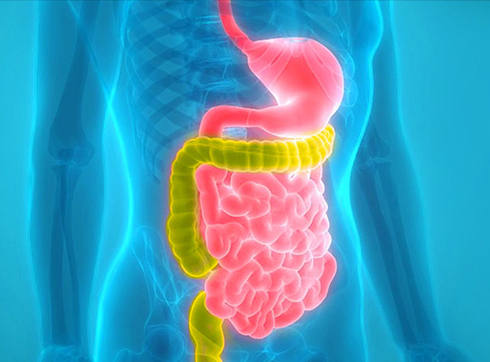
Clinical presentation
The disease is characterized by a long asymptomatic course, making timely diagnosis difficult. Clinical manifestations become noticeable primarily when the tumor has significantly grown and spread beyond the pancreas.
Early symptoms
The initial stage of the disease often masquerades as common gastrointestinal disorders. Pain is present, but intermittent and subtle. Patients in the early stages of cancer may also experience:
- Unexplained weight loss while maintaining a normal diet
- Occasional discomfort in the epigastric region
- Periodic pulling sensations in the lumbar region
- Changes in food preferences with an aversion to fatty foods
- Dyspeptic symptoms: flatulence, nausea, irregular bowel movements
The patient's general condition is often accompanied by unexplained weakness, apathy, and decreased performance.
Late symptoms
As the cancer progresses, the clinical picture becomes more pronounced and specific.
- Mechanical jaundice develops: the skin, sclera, and mucous membranes take on an intense yellowish tint, urine darkens, and stools become acholic (discolored). This process is accompanied by debilitating itching.
- Pain intensifies, becoming constant and excruciating, especially if the tumor invades the nerve plexuses.
- Cancer intoxication develops, leading to severe cachexia (wasting) and persistent fever.
- Metastasis to the peritoneum can lead to ascites—fluid accumulation in the abdominal cavity.
- The risk of thrombosis increases. In particular, there is a high risk of developing migratory thrombophlebitis (Trousseau's sign). A sign of this condition is the appearance of painful redness and hardening along the veins in various parts of the body, which may disappear on their own and then reappear.
- If the endocrine part of the organ is affected, secondary diabetes mellitus may manifest. This is characterized by sudden intense thirst, dry mouth, and increased urine output.
Any of these symptoms is a serious reason to immediately consult an oncologist.
Diagnosis of pancreatic cancer
The difficulty of early detection is due to the long asymptomatic development of the pathology. By the time pronounced clinical symptoms appear, the tumor process often reaches a widespread stage with metastasis. Modern pancreatic cancer diagnostics requires a comprehensive approach using laboratory and instrumental techniques.
Laboratory diagnostics
Laboratory diagnostics provide valuable information about the functional state of the pancreas and systemic changes in the body characteristic of oncology. Blood and biological fluid tests can identify specific markers indicating the presence of a pathological process. The following are used to diagnose cancer:
- Blood tests for pancreatic enzymes, bilirubin metabolism parameters, and liver function tests
- Tumor marker testing, particularly CA 19-9, although its specificity requires further confirmation.
- Coagulation profile evaluation to identify associated disorders
- Molecular genetic testing to determine targeted therapy tactics
- Liquid biopsy – detection of circulating tumor cells and DNA in the blood
Instrumental diagnostics
Visualization of pancreatic structures and surrounding tissues is a key step in confirming the diagnosis. Modern instrumental methods allow us to accurately determine the location, size, and nature of the tumor, as well as assess the extent of the process.
The patient undergoes:
- Abdominal ultrasound is a basic screening diagnostic method for primary complaints.
- Endoscopic ultrasound (endosonography) provides detailed visualization of the pancreas and allows for fine-needle biopsy.
- Contrast-enhanced computed tomography determines the size, location, and relationship of the tumor to surrounding structures.
- Magnetic resonance imaging with cholangiopancreatography protocols (MRCP) provides detailed information about the condition of the pancreatic and bile ducts.
- ERCP combines endoscopic and radiological methods, allowing for tissue collection and stent placement.
- PET-CT detects distant metastases and Assesses the extent of the process.
- Angiography – determines the characteristics of the tumor's blood supply and its relationship to the main vessels.
For a definitive diagnosis, histological confirmation of the malignancy of the tumor is required by biopsy, performed under ultrasound or CT guidance.

Post-treatment rehabilitation
Comprehensive recovery after aggressive anticancer treatment is a multi-stage process requiring an integrative approach. A medical rehabilitation program is developed individually, taking into account the extent of the intervention, the patient's age, and the patient's functional state.
- Post-Surgical Recovery. Post-operative rehabilitation includes early patient activation to prevent thromboembolic complications and pneumonia. A special kinesitherapy program is aimed at restoring abdominal muscle strength and preventing post-operative hernias. Breathing exercises and postural drainage help improve pulmonary ventilation. Gentle physiotherapy procedures help relieve pain and normalize gastrointestinal motility.
- Nutrition support and diet therapy. A specialized diet includes frequent meals with increased levels of easily digestible protein and limited fat. Synthetic nutritional mixtures for enteral nutrition are prescribed if necessary. Lifelong pancreatic enzyme replacement therapy is a mandatory component of rehabilitation measures, the dosage of which is individually determined based on a coprological examination and nutritional status assessment.
- Immunity strengthening. Immunomodulatory support after pancreatic cancer is aimed at restoring adaptive immunity and preventing the development of infections. It includes the use of prebiotics, vitamin and mineral complexes, and specialized metabolites.
- Psychiatric care. Psychotherapeutic support is aimed at overcoming anxiety and depressive disorders associated with the disease. Cognitive behavioral therapy helps adapt to a new quality of life, while relaxation techniques reduce stress. If necessary, mild antidepressants with minimal side effects are prescribed. Self-help groups and social integration contribute to the improvement of psycho-emotional well-being.
The rehabilitation program is implemented under the constant supervision of a multidisciplinary team of doctors, including an oncologist, nutritionist, physiotherapist, and psychologist. Regular assessment of the effectiveness of rehabilitation measures allows for timely adjustments to the strategy and optimal results.
FAQ
Which modern approaches are the most promising?
Which diagnostic methods provide the greatest accuracy?
How effective is surgical treatment?
Where should I go for pancreatic cancer treatment in Moscow?
Our doctors

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Price
Other services






































































About the disease
The pancreas is located in the left upper quadrant near the stomach and duodenum. It is penetrated by excretory ducts, vessels, and nerves, covered by a connective tissue capsule, and consists of three parts: the head, body, and tail. The excretory duct joins the bile duct at the head of the pancreas and opens into the duodenum.
What is the pancreas?
The main function of this organ is to produce pancreatic juice, rich in digestive enzymes (amylase, lipase, protease). These substances enter the lumen of the duodenum, where they actively break down complex protein, fat, and carbohydrate molecules into smaller compounds, ensuring normal digestion. At the same time, special cell clusters—the islets of Langerhans—produce vital hormones: insulin and glucagon. These are directly released into the blood and regulate carbohydrate metabolism, maintaining optimal glucose levels. Thus, the pancreas is an indispensable component of both the digestive and endocrine systems.
As cells divide, mutations can occur, and some of these mutations can disrupt the functions that control cell division. Then, the cells begin to divide uncontrollably, forming a tumor.
Pancreatic cancer is one of the most aggressive types of cancer. It often remains asymptomatic until the late stages of the disease, when treatment becomes very difficult. Cancer cells can spread throughout the body through the bloodstream, forming distant secondary tumors (metastases).
The five-year survival rate (the percentage of patients who survive five years after diagnosis) for early-stage pancreatic cancer is up to 15%. This is because the organ is located in a difficult-to-reach place for surgery and is closely surrounded by other organs. Surgeons must be highly experienced in performing malignant tumor removal procedures. The risk of complications after surgery is very high.
Pancreatic cancer is the sixth most common cancer and accounts for 7% of cancer deaths of all types. It most often affects older adults of both sexes. In more than half of cases, the tumor develops in the head of the pancreas. And in almost a third of cases, the entire organ is affected.
Get examined at our clinic to quickly detect diseases of the pancreas and other organs.