Treatment of oncology (tumors, cancer) of the lung and mediastinum
Lung cancer is a malignant neoplasm that develops from the epithelial cells of the bronchi or lung tissue. It is one of the most aggressive oncological diseases, ranking first among cancer deaths worldwide.
Lung cancer claims more than 1.8 million lives annually worldwide. Late diagnosis is a particular danger. In 70% of patients, the disease is diagnosed at stages III-IV, when radical treatment is no longer possible. Rapid metastasis to the brain, bones, and liver is particularly problematic, significantly worsening the prognosis.
The K+31 Clinic in Moscow employs highly qualified doctors who use advanced lung cancer diagnostic methods, allowing for the detection of pathologies in the early, asymptomatic stages.

specialists
equipment

treatment
Causes and risk factors
The main cause of lung cancer is smoking, including passive smoking. Chemical carcinogens in cigarettes damage the DNA of respiratory tract cells, triggering their malignant transformation.
The following factors also increase the risk of lung cancer:
- Poor environmental conditions: industrial emissions, exhaust gases, radon
- Occupational hazards: exposure to asbestos, heavy metals, coal dust
- Unfavorable heredity
- Chronic lung diseases
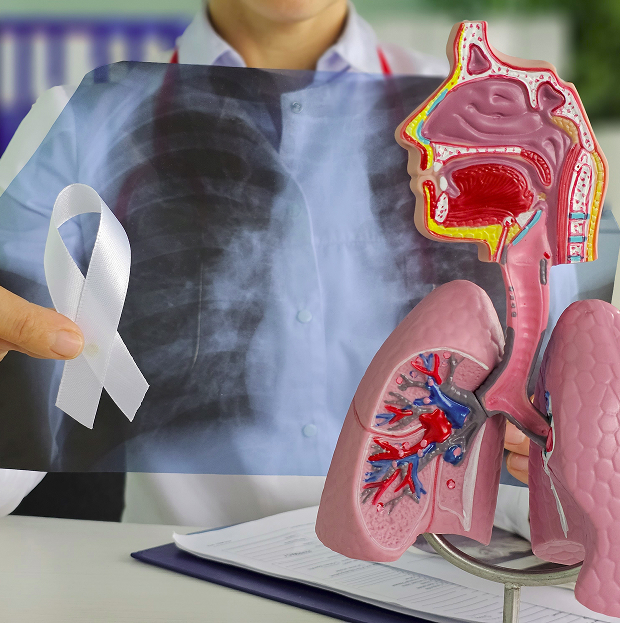
Risk factors for developing lung cancer
It is known that the main risk factor for lung cancer is the inhalation of carcinogens. Approximately 90% of identified cases are associated with smoking, or more precisely, with exposure to carcinogens contained in tobacco smoke. The risk increases proportionally to the length of a smoker's life and the number of cigarettes they smoke. That is, the longer a person smokes and the more cigarettes (or packs of cigarettes) they smoke per day, the higher the risk. For a smoker, the most effective way to reduce the risk of developing the disease is to quit.
Not only smokers are at risk, but also those around them. Passive smoking is also a risk factor. For example, in a married couple where one smokes and the other does not, the non-smoker's risk of developing lung cancer increases by 30%.
Smoking is the main cause of the disease, but not the only one. Air pollution also provokes it. Residents of industrialized areas with manufacturing and mining industries are 3-4 times more likely to develop lung cancer than people living in rural areas. Other risk factors include:
- Radiation exposure
- Long-standing, untreated lung diseases, such as tuberculosis, bronchitis, pneumonia, and bronchiectasis
- Exposure to certain substances: asbestos, arsenic, cadmium, nickel, radon, chloromethyl ether, and chromium

Symptoms and early manifestations
The main symptoms of lung cancer are:
- A persistent cough (more than 3 weeks) that does not respond to standard treatment
- Blood in the sputum
- Shortness of breath that worsens with physical exertion
- Chest pain that worsens with deep breaths
- Unexplained weight loss (5-7 kg per month)
- Weakness, increased fatigue
Lung cancer can develop asymptomatically for a long time, making early diagnosis difficult.
Worrying signs requiring urgent examination:
- Recurring pneumonia in the same lung lobe
- Swollen lymph nodes above the collarbone
- Hoarseness without signs of a cold

Clinical picture of lung cancer
The clinical presentation of lung cancer is "hidden" and nonspecific, i.e., characteristic of various respiratory diseases. This is why, when it appears, many people hesitate to get tested. They underestimate the severity of the problem. In the early stages of the disease, increased fatigue, a slight decrease in performance, interest in life, and apathy are observed. This should alert everyone. Other symptoms include:
- Difficulty breathing
- A persistent, prolonged cough
- Chest pain or discomfort
- Progressive shortness of breath
- Blood-tinged sputum
- Hoarseness
- Loss of appetite
- Unrelated weight loss
- Progressive fatigue
- Swelling of the face or swollen veins in the neck
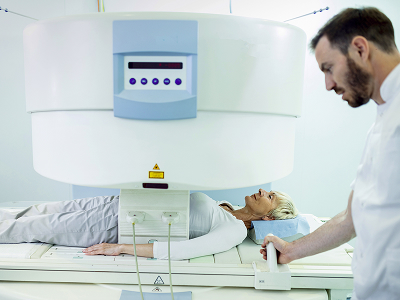
How is lung cancer diagnosed?
A range of modern methods are used to diagnose lung cancer:
- Computed tomography (CT): the primary method of tumor visualization, allows determining the size, location, and structure of the tumor.
- PET-CT: helps identify metastases and assess the extent of the pathological process.
- Biopsy: collecting a tissue sample for histological examination.
- Sputum cytology: indicated to detect atypical cells.
- Laboratory testing for tumor markers.
The primary method for diagnosing lung cancer in oncology is computed tomography. Tomography. If a tumor is detected in a patient, a series of additional tests are prescribed to determine the type of tumor. If it is malignant, the type of cancer and its extent will be determined. Bronchoscopy plays an important role among additional diagnostic methods. In some cases, it can detect carcinoma protruding into the bronchial lumen, infiltration, or compression of the bronchial walls.
During a bronchoscopy, a thin, flexible tube with a lens at the end is inserted into the patient's bronchus. It can be used to visually determine the presence or absence of cancer symptoms and to collect a biopsy sample. This sample is needed for subsequent testing. If the case is diagnostically unclear, the treating physician may decide to resect the area of the lung where malignancy is suspected. These methods provide reliable information about the presence of tumor changes, their extent, and the stage of the disease. Based on this information, a cancer treatment regimen is selected.
Positron emission tomography combined with computed tomography (PET-CT) is the gold standard in lung cancer diagnostics due to the following capabilities:
- High accuracy (up to 95%) in detecting metastases
- Early detection of tumors as small as 4-5 mm
- Qualitative assessment of tumor activity
- Ability to distinguish malignant from benign tumors
- Assistance in assessing the effectiveness of cancer treatment
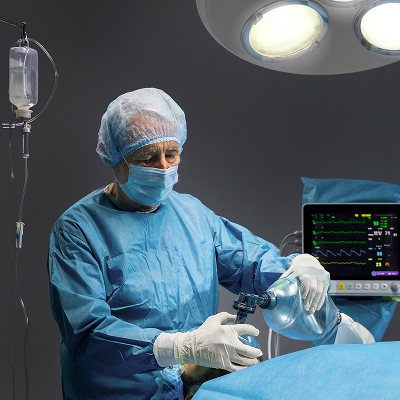
Treatment methods
Lung cancer treatment involves surgical removal of the tumor, drug therapy (chemotherapy, targeted therapy, and immunotherapy), radiation therapy, and various combinations of these. The choice of a specific method depends on the patient's condition, the stage of the disease, the size of the tumor, and other factors. Surgery is the most effective cancer treatment. During surgery, either the portion of the lung containing the tumor or the entire lung along with regional lymph nodes is removed. The outcome of the surgery depends on the location and size of the tumor, the patient's age, and the presence of metastases.
The second most effective treatment for lung cancer is radiation therapy. This method uses ionizing radiation to target the tumor. High efficiency is achieved through the use of modern equipment (VARIAN linear accelerators with a 3D planning system) and work in accordance with international standards. Chemotherapy involves the administration of drugs that selectively suppress the growth of malignant cells. This method does not cause serious damage to healthy organs and tissues.
Chemotherapy is the primary treatment for tumors and advanced cases of lung cancer.
In recent years, immunotherapy has become a prominent component of oncology, alongside chemotherapy and targeted therapy, in the treatment of lung cancer. Immunotherapy has revolutionized the treatment of patients with this serious disease. Immunotherapy drugs significantly increase life expectancy and can cure approximately one in six patients with late-stage lung cancer! In fact, chemotherapy without immunotherapy should no longer be used.
Surgical treatment is typically used in the early stages of cancer, particularly for localized, non-small cell tumors. But only if the patient's condition allows for such surgery. At later stages, surgical removal of the tumor is ineffective. These cases are characterized by a large tumor size, the presence of metastases in distant organs and regional lymph nodes. Surgery is also not used for small cell lung cancer. If surgery is contraindicated, chemotherapy and radiation therapy can help. Comprehensive cancer treatment, including all the methods described above, is performed if the patient's condition allows it.

Since smoking is the leading cause of lung cancer, the best prevention for non-smokers is to avoid this dangerous habit, and for smokers, to quit. It's also important to protect yourself as much as possible from other harmful influences, such as air pollution from automobiles and industrial emissions, household exposure to radon, and exposure to industrial carcinogens. When combined, smoking and other risk factors are mutually reinforcing. Secondary prevention is also important, including annual screening for people at high risk. This allows for the detection of lung cancer at an early stage, when the disease is curable.

In oncology, mediastinal cancer refers to all malignant tumors of the mediastinum—that is, the organs located in the chest cavity between the lungs. These organs in the mediastinum include the thymus gland, esophagus, trachea, heart, aorta and other blood vessels, lymph nodes, and nerves. These tumors are also called mediastinal tumors. In most cases, they are benign. Malignant tumors (when a patient is diagnosed with mediastinal cancer) occur in 40% of cases.
The most common forms of mediastinal cancer are lymphoma, neuroblastoma, thymoma (thymus cancer), chondrosarcoma, angiosarcoma, dysgerminoma, osteoblastosarcoma, as well as metastases from melanoma, lung cancer, breast cancer, esophagus cancer, and others.
The causes of mediastinal tumors are not fully understood. Risk factors include ionizing radiation, carcinogens, and certain viruses (HIV, Epstein-Barr virus, etc.). Mediastinal tumors are relatively rare, but the occurrence of malignant tumors in the chest is weakly related to the patient's age and gender, and they can develop from any tissue or organ in the mediastinum.
What do we treat
Classification
By location, mediastinal tumors in oncology are classified as: anterior (germ cell tumors, lymphoma, thymoma), central (lymphadenopathy, esophageal or tracheal tumors), and posterior mediastinal (neurogenic tumors, lymphadenopathy).
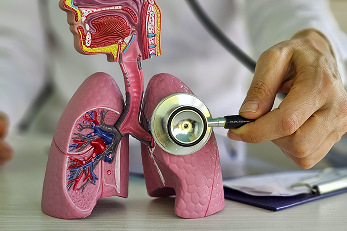
Mediastinal cancer is divided into:
- Primary Mediastinal tumors arising in the tissues of the mediastinum itself or in the tissues bordering the mediastinum: neurogenic tumors, fibrosarcomas, lymphomas, thymomas, liposarcomas, etc.
- Secondary Metastases of mediastinal tumors from adjacent chest organs

Symptoms of the disease
Until a mediastinal tumor reaches a certain size, the cancer is asymptomatic, with no clinical manifestations. Symptoms appear as the tumor grows. Malignant mediastinal tumors can grow quite rapidly, so the transition from the asymptomatic stage to a pronounced clinical picture can be short.
As the tumor grows, it begins to put pressure on or invade adjacent organs, which can cause:
- Chest pain radiating to the neck, shoulder blade, or shoulder
- Shortness of breath if the tumor presses on the trachea and bronchi
- Difficulty passing food through the esophagus due to compression of the esophagus
- Bluish discoloration of the face or a heavy head due to compression of a vein
- Redness of the face if the tumor presses on nerves
Other symptoms and signs of mediastinal cancer may include: cough, hoarseness, fever and sweating, chest pain, hypoglycemia, muscle weakness, itching, dilated veins of the face or neck, Heart rhythm disturbances, weight loss, etc.
The clinical picture depends on the location and nature of the mediastinal tumor (benign or malignant) and its growth rate.
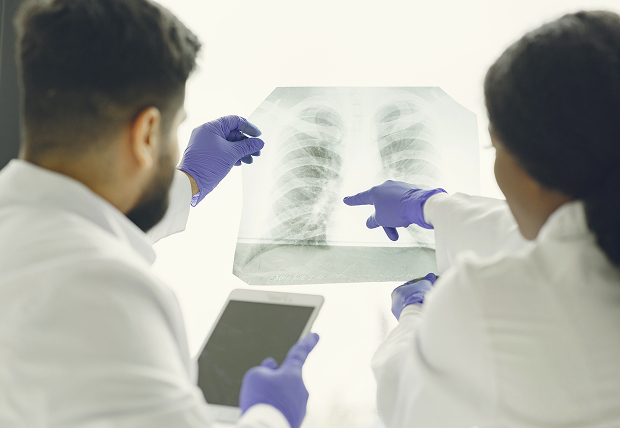
How is mediastinal cancer diagnosed?
Imaging methods such as chest X-ray and CT scan can be used to detect mediastinal tumors. X-ray is the primary method for detecting mediastinal cancer. CT scans can determine the tumor's location and extent.
After visual detection of a tumor, a definitive diagnosis is made by histological verification—a biopsy—either transbronchial (mediastinal tumor cells are collected via bronchoscopy) or transthoracic (collected via a chest puncture during ultrasound or CT).
Mediastinoscopy and video-assisted thoracoscopy are also used to diagnose mediastinal cancer, along with other additional tests.
Treatment methods
Treatment for mediastinal cancer depends on the location, origin, histological type, and size of the mediastinal tumor. This may include:
Surgical treatment (removal)
This is a rather complex procedure, given the close proximity of vital organs in the mediastinum. It is often performed after a course of chemotherapy or radiation therapy, or even after several courses of chemotherapy. This treatment is used for thymomas and neurogenic tumors of the mediastinum.
Chemotherapy
It is often used as adjuvant therapy to shrink a malignant mediastinal tumor before its removal or to prevent recurrence after surgical removal. In some cases, chemotherapy is used as maintenance treatment for mediastinal cancer when surgery is not possible, to slow the growth of cancer cells and improve the patient's condition. Chemotherapy is used to treat lymphomas and some other types of mediastinal cancer.
Radiation therapy
Like chemotherapy for cancer, it is used in conjunction with radical treatment (surgery), before or after surgery to remove residual malignant cells, or as a palliative treatment to eliminate complications. Radiation therapy is used to treat lymphomas, teratomas, thymomas, and other types of mediastinal cancer.
Since the cause of mediastinal tumors is unclear, it's difficult to discuss preventative measures. However, the earlier cancer treatment begins, the more optimistic the prognosis for recovery. Therefore, if the above symptoms persist for more than 10 days, it's worth consulting your doctor for diagnosis and early treatment of mediastinal tumors.
Our doctors
Make an appointment at a convenient time on the nearest date
Price

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Other services
Reviews






































What is the danger of lung cancer?
Lung cancer is a malignant tumor that develops from the lung parenchyma or bronchial tissue. This type of cancer is one of the most common oncological diseases. It is characterized by early metastases and an insidious progression, meaning it is not accompanied by obvious symptoms. As a result, the disease is often detected at stages 3 or 4. This is where its danger lies.