Diagnosis, Treatment, and Removal of Skin Melanoma
Melanoma is one of the most aggressive malignant skin tumors, prone to rapid progression and early metastasis. However, timely diagnosis dramatically improves the prognosis: detecting a tumor at stages I–II allows for stable remission. The K+31 Clinic offers comprehensive examinations using modern equipment, including dermatoscopy and digital nevus mapping, and employs advanced surgical and therapeutic treatment methods.

specialists

equipment

treatment
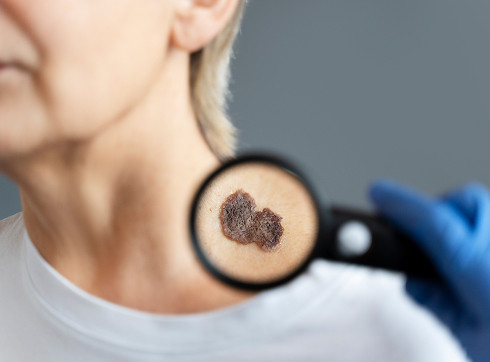
What is melanoma?
Melanoma is a malignant tumor that affects the skin, mucous membranes, and even the retina. Melanoma is characterized by aggressive tumor growth. It is formed from melanocytes and melanoblasts—melanin-containing cells that also form moles.
Melanoma is considered one of the most dangerous types of cancer due to its asymptomatic and rapid progression, its metastasis and frequent relapses, and its weak immune response. Other skin tumors grow more slowly and metastasize less frequently.
Melanoma cancer cells actively divide and penetrate deep into the skin, from where they spread to the lymph nodes and internal organs. This is why melanoma is considered one of the most dangerous skin tumors. Call us or schedule an appointment online for timely diagnosis and high-quality treatment in Moscow.

Classification of Malignant Tumors
Scientists have developed a special classification of melanoma to better understand the characteristics of its different types. Each type of pathology has its own characteristics, behavior, and treatment methods.
Melanoma is classified based on its growth patterns and clinical manifestations. Let's take a closer look at the main types of this malignant tumor.
Superficial Spreading
This type of melanoma initially grows horizontally, spreading across the surface of the skin. Initially, the tumor appears as a flat spot, then begins to deepen and develop into a nodule.
Malignant Lentigo
This melanoma develops from lentigo spots, which resemble large, dark freckles. The malignant tumor begins as a flat spot, then begins to rise above the skin's surface.
Acral-lentiginous
This type of melanoma is rare and most often localized on the palms of the hands, soles of the feet, and nail beds. Acral tumors appear as dark spots, later acquiring irregular outlines.
Nodular
This type of melanoma is characterized by its initial vertical growth, forming a nodule or tubercle. Nodular tumors are characterized by rapid growth and a high risk of metastasis.
Causes and risk factors

Melanoma, a serious disease that manifests as a malignant skin tumor, develops for a variety of reasons. Numerous risk factors have been identified that increase the likelihood of developing this dangerous disease. Knowing these factors can minimize the risk of developing this pathology.
To understand the mechanism of melanoma development, it's important to understand what can influence the state of the melanocyte pigments that make up the malignant tumor. These pigments are responsible for skin color and tanning. Small skin growths that are overflowing with these pigments are called moles, or nevi. Under certain factors, nevi can become malignant, their cells multiplying uncontrollably, forming a tumor and metastasizing.
Causes of Melanoma Development
Factors that trigger malignant transformation of moles can include excessive ultraviolet radiation, thyroid or endocrine diseases, and trauma to the moles.

These tumors can vary in size, shape, and texture. Melanoma can occur in various locations: lips, eyelids, other parts of the face, scalp, neck, limbs, and torso. Melanoma does not develop from a single cause, but from a combination of factors. External factors, such as sun exposure, interact with internal factors such as immune system strength, genetic predisposition, and overall health.
Each individual factor alone cannot cause the disease, but a combination of factors creates favorable conditions for the development of melanoma. Risk factors for developing malignant tumors include:
- Sunburn, tanning beds
- Genetic predisposition
- Frequent exposure to carcinogens and toxins
At-risk groups include the elderly and people with fair skin, freckles, and red hair. These individuals also work in hazardous environments. These individuals should undergo regular examinations and pay closer attention to moles, freckles, and any changes in them.

Ultraviolet Radiation
Sun exposure and tanning beds significantly influence the development of melanoma. Ultraviolet radiation damages the DNA of skin cells, triggering mutations and the transformation of healthy cells into cancerous ones.
Phenotype
Scientists have proven that people with fair skin are much more likely to develop melanoma. This is because fair skin is less protected from sun radiation, which increases the risk of developing the disease.
Number of Moles
A large number of moles increases the risk of melanoma. Atypical moles of irregular shape or color are especially dangerous. The more moles there are, the higher the risk of developing cancer.
Genetic Predisposition
Genetics plays a significant role in the development of melanoma. If close relatives have had melanoma, the risk of developing the disease increases significantly.
Other factors
Chemicals and poor environmental conditions are also significant causes of melanoma. Chemicals irritate the skin, lead to inflammation, and increase the risk of cell degeneration.
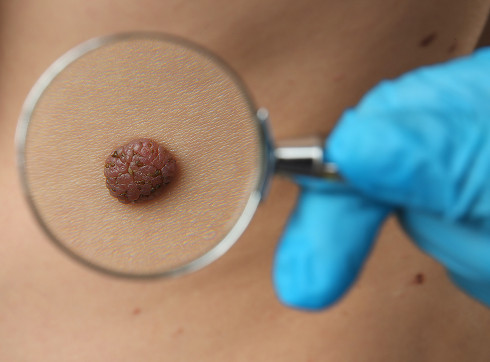
Melanoma Symptoms
The main danger of this malignant tumor is that melanoma can develop and show no symptoms for a long time; the clinical picture is not clearly visible in the early stages. Often, the cancerous process develops asymptomatically in the superficial layers of the skin for several years, and then suddenly begins to spread through the bloodstream and lymph to other organs—the brain, lungs, liver, lymph nodes, and so on. There, new foci of cancer cell growth—metastases—begin to form.
Melanoma skin cancer often appears as a flat, painless lesion or nodule on the skin. Its color can be brown, pink, or blackish-blue. In some cases, the tumor takes on multiple shades due to uneven pigment distribution (a similar pattern can occur with a non-cancerous birthmark). However, overall, the clinical picture varies.
Non-ulcerating melanoma typically has a relatively favorable course. In the case of a nodular form and the presence of ulceration, there is a higher risk of developing metastases.
You should pay attention to the following symptoms:
- The mole's furrows have disappeared, and its surface has become smooth
- The mole has increased in size
- Unpleasant sensations, burning, itching, and pain have appeared in the area of the tumor, the degree of which depends on the stage of the disease and its severity
- The mole has become dry and flaky
- It is bleeding, there are ulcers
- There is redness in and around the mole, as with inflammation
- "Daughter" moles have appeared
- Hair loss in the area of the tumor
- Nearby lymph nodes have enlarged
- Loss of appetite, a sharp decrease in Weight
The first signs of melanoma that should raise concern include symptoms such as a raised tumor, irregular edges, asymmetry, uneven color, a diameter greater than 6 mm, rapid growth, and changes in color and/or structure. If the initial symptoms of the disease are ignored, it progresses, revealing new warning signs.
The tumor increases in size, changes shape, and changes color. The edges of the skin cancer become uneven, and the surface becomes bumpy or ulcerated. The neoplasm may become covered with small nodules, plaques, or ulcers. This is dangerous because such changes indicate aggressive disease progression. The skin around the lesion becomes red, swollen, and itchy. The color of the mole itself becomes uneven—various shades of brown, black, red, and blue may be present simultaneously.
Early and Late Signs of Melanoma
Self-examination of your skin is an important step in the fight against melanoma. Regular self-diagnosis helps you spot suspicious signs early and consult a specialist. Melanoma develops rapidly, but may not cause any symptoms at first. It's important to remember that every minute of delay increases the risk of complications.
How is melanoma different from a benign mole?
Regular self-examination of your skin—a visual inspection—can help you identify suspicious growths in the early stages. There are a number of signs of mole degeneration (the so-called "melanoma ABCs"), marked with the first letters of the Latin alphabet:
- A (asymmetry)—asymmetry. Harmless nevi and benign tumors often have a symmetrical shape.
- B (border irregularity)—irregular borders. Unchanged moles have smooth, defined edges. Melanoma, on the other hand, typically has an uneven, "blurred" outline.
- C (color) – color. If it's a benign lesion, it will have a relatively uniform color. However, if a mole has differently colored parts, this may indicate malignant transformation.
- D (diameter) – diameter. A non-pathological nevus typically doesn't exceed 6 mm in diameter. A larger diameter may indicate melanoma transformation. In any case, any changes in a pre-existing mole may indicate malignancy. Numerous observations have shown that pigmented lesions that frequently changed color and shape were four times more likely to be melanoma than moles that remained unchanged. In view of this, a fifth letter was subsequently added to the four letters of the "melanoma alphabet."
- E (evolving) - changes. Signs of melanoma that should raise alarm include the following manifestations: change or absence of skin pattern at the site of the nevus, an area of scaling or the so-called "varnish" surface; change in the color of the nevus, which suddenly became excessively pigmented or, conversely, lost its original shade; blurring of the contour; a sensation of tingling, itching, burning at the site of the mole; redness around the formations, indicating inflammation; an increase in the size of the nevus, its hardening (especially in patients over 30 years of age); cracks, ulcers, bleeding of the nevus; disappearance of the mole (this should be especially alarming if this occurred after tanning in a solarium or in the sun); Hair loss from the mole.
This symptom—any changes in the mole—is the most critical. If the mole is noticeably growing and changing, it is most likely melanoma.
Remember that all of these symptoms and signs of melanoma are for informational purposes only. Diagnosis should only be made by your doctor (and not by yourself), especially in the case of skin melanoma, one of the most aggressive types of cancer.
A, asymmetry
If one side of a mole is noticeably different from the other, this is the first reason to consider the possibility of melanoma. Asymmetry is not a good sign.
B, borders
The borders of a healthy pigmented spot are clearly defined. Irregular, blurred, or jagged borders may indicate the development of melanoma.
C, color
Any differences in color—the presence of different shades of brown, gray, white, or even a bluish tint—are a sign of possible melanoma.
D, diameter
A healthy mole rarely exceeds 6 millimeters in size. Larger sizes are a significant risk factor for melanoma.
E, evolving
Any change in an existing mole—whether in shape, color, size, or the development of itching, bleeding, or flaking—may indicate the development of melanoma.
Melanoma Stages
Understanding the stages of melanoma is important to understand how far the disease has progressed. The stage indicates the depth of tumor penetration and whether it has spread to lymph nodes or other organs. The earlier the correct stage of cancer development is determined, the more effective the treatment and the higher the chance of a full recovery. For convenience, three types of melanoma and four stages of disease development have been developed.
Clinical Classification and Staging of Melanoma
Melanoma skin cancer is divided into three types:
- Superficial spreading melanoma is the most common. It has an irregular shape, jagged edges, and a brownish, uneven color. The tumor may discharge, and the melanoma may bleed. It grows superficially (radial growth phase) and deeper into the tissue (vertical growth phase), with the transition to the growth phase lasting months or years.
- Nodular melanoma is the most aggressive type of skin cancer. It develops from both pigmented nevus and normal skin. The tumor rapidly grows vertically above the surrounding tissue and has a uniform dark blue or almost black color. In rare cases, melanoma may be non-pigmented.
- Malignant lentigo is rare and usually occurs in the elderly. It appears as small (up to 3 mm) nodules on exposed areas of the body (arms, neck, face). It is dark blue or dark and light brown in color. It grows slowly and sometimes invades follicles.
Melanoma classification is important for understanding the severity of the disease and choosing the right treatment. Four stages of pathology development characterize the depth of tumor penetration and the spread of cancer cells throughout tissue.
Stage 0
At this stage, the melanoma is located within the top layer of the skin ("in situ").
Stage I
Tumor cells are localized (in the outer layer of the skin). At this stage, the melanoma reaches a thickness of 1–2 mm.
Stage II
The skin cancer begins to grow deeper (up to 2 mm), ulcers appear on the tumor, and the melanoma may begin to bleed. At this stage, the melanoma becomes larger and more aggressive. The risk of recurrence increases.
Stage III
Cancerous cells have spread to the lymph nodes closest to the tumor. At this stage of melanoma development, the prognosis worsens.
Stage IV
At this stage, melanoma causes metastases that spread throughout the body, affecting distant organs. The tumor invades other areas of the skin, metastases penetrate organs and tissues, and spread through the blood and lymph.
The deeper the melanoma tumor penetrates into the dermis, the higher the likelihood of metastasis. There are five levels of penetration, with level 1 being non-invasive and level 5 being the tumor that has reached the subcutaneous fat.
Correctly determining the stage of skin cancer is crucial for choosing a treatment plan.
What do we treat
Our doctors

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Price
Other cancer treatment services







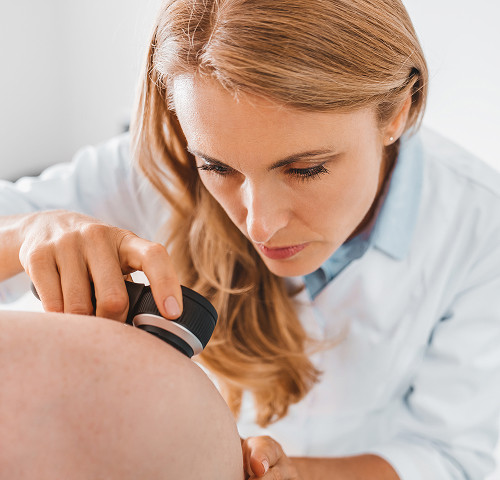

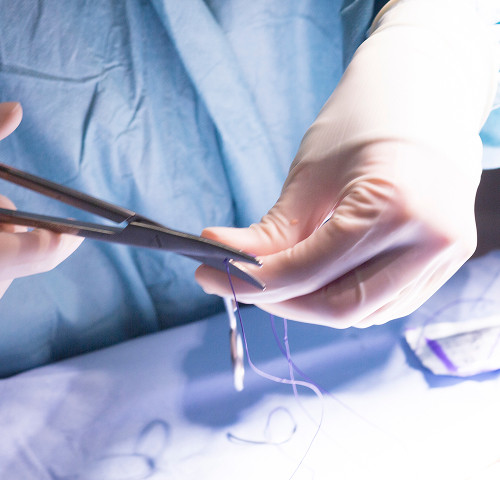















































































Definition and classification of melanoma
A dangerous tumor called melanoma occurs on the skin, mucous membranes, and even the eyes. This malignant pathology is a type of cancer. It develops from cells that produce the pigment melanin, which is what makes up our moles.
The main problem with melanoma is its rapid growth and ability to spread metastases throughout the body undetected. This is why, if you suspect this cancer, it is so important to see a doctor promptly and undergo a thorough diagnosis.