Plaster Casting for a Child: The Procedure, Types of Casts, and Care
Child injuries are common. If a child is diagnosed with a serious childhood injury, doctors need to immobilize the broken bone. Immobilization is one of the main treatment methods, allowing the bone structures and ligaments to return to their proper position.

specialists

equipment

treatment
How is a plaster cast applied?
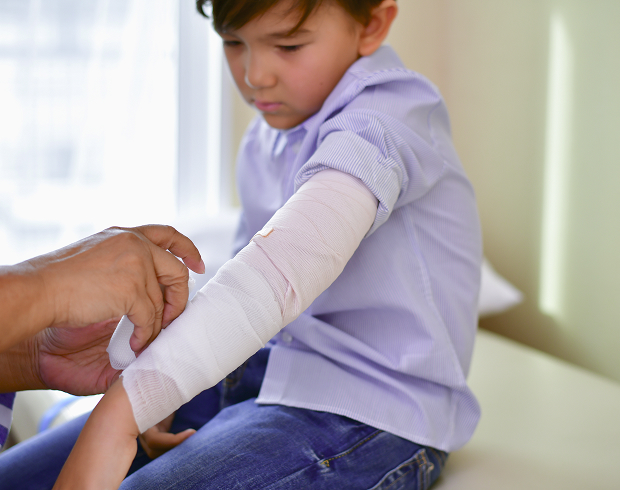
The procedure for applying fixation materials is meticulously developed to minimize patient discomfort and ensure maximum precision.
Examination and diagnostics before immobilization
Before immobilization, the doctor performs clinical tests: checking sensitivity, vascular pulsation, and range of motion. An X-ray is a mandatory step. These images allow the precise fracture line to be visualized and determine whether reduction (alignment of the fragments) is necessary before casting.
Preparing the child for the procedure
Preparation includes hygienic preparation of the skin, unless there are open wounds. If there are abrasions, they are treated with antiseptics. To protect the skin from pressure and rubbing, a soft knitted underlayer or a special cotton pad is applied to the limb beforehand.

Applying a Plaster Cast and Monitoring Limb Position
The process itself involves layering wet bandages soaked in a plaster mixture. The doctor positions the limb in a physiologically correct position. While the cast hardens, the pediatric traumatologist holds the limb with their hands, preventing displacement. It is important that the immobilization of the limb be sufficiently tight, but not disrupting circulatory control.
What does the child feel during the procedure?
As the plaster hardens, a chemical reaction occurs, releasing heat. The child may feel a pleasant warmth. The procedure itself is painless; however, if bone reduction was performed, a nagging pain may persist, which gradually subsides after immobilization.
Types of plaster casts for children
Depending on the severity of the injury and the stage of treatment, different designs are used.
Circular plaster cast
This is a classic "closed" cast that completely encircles the limb. This type of cast provides the most rigid fixation. It is usually applied at later stages, when the initial post-traumatic swelling has begun to subside, to avoid tissue compression.
Splint
A splint is a strip of plaster that covers the limb on only one or both sides and is secured with a soft bandage. This is the safest option for the first few days after an injury. It allows the cast to expand along with the swollen tissue without disrupting blood flow.
Removable immobilization and alternative options
Minor ligament injuries are treated with a removable cast. This makes it easier to shower and return to an active lifestyle.
What are the differences between modern materials?
Today, in addition to regular plaster casts, immobilization with polymer bandages ("plastic cast") is used.
| Type of fixation | When used | Advantages | Important features |
|---|---|---|---|
| Circular cast | For injuries requiring rigid fixation | Reliable immobilization | Requires swelling control |
| Splint | At the initial stage of treatment | Easier to take swelling into account | Can be a temporary solution. |
| Removable fixation | During the recovery phase | More comfortable for the child | Use only as prescribed by a doctor. |
Modern polymers are several times lighter, are moisture-resistant (with a special lining), and allow the skin to ventilate better, which is critical in the summer.
FAQ
How do you know if your child needs a cast?
How long does a child wear a cast?
Can a plaster cast get wet?
When should I see a doctor immediately after a cast is applied?
Our doctors

This award is given to clinics with the highest ratings according to user ratings, a large number of requests from this site, and in the absence of critical violations.

This award is given to clinics with the highest ratings according to user ratings. It means that the place is known, loved, and definitely worth visiting.

The ProDoctors portal collected 500 thousand reviews, compiled a rating of doctors based on them and awarded the best. We are proud that our doctors are among those awarded.
Make an appointment at a convenient time on the nearest date
Price
Other Services








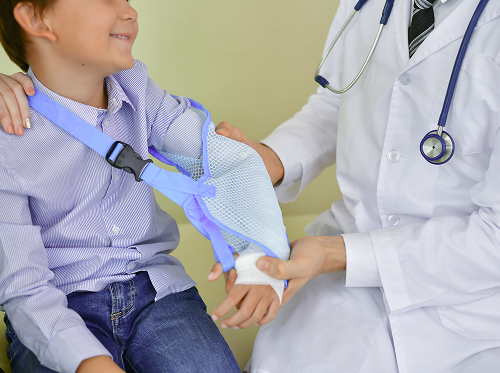




































When does a child need a cast?
The decision regarding the need for a plaster cast is made exclusively by a pediatric traumatologist. This is based on the results of an examination and instrumental diagnostics. The main goal of fixation is to provide complete rest to the injured area to prevent displacement and accelerate healing.
Fracture, crack, and dislocation: What's the difference?
A fracture in a child differs from an adult fracture. Due to the thick periosteum, the bone often breaks in a "greenstick" pattern—an internal fracture while the outer shell remains intact. A crack in the bone is considered an incomplete fracture, but it also requires strict mobility restriction. A dislocation, on the other hand, involves the protrusion of the joint head from the socket. After its reduction, doctors apply a cast to allow the damaged ligaments and joint capsule to heal without stretching under the weight of the limb.
What injuries most often require immobilization?
In medical practice, plaster casts are most often applied to children with injuries to the tubular bones. Statistically, the following areas are most often used:
Symptoms that require consultation with a traumatologist
A child may not always be able to clearly describe their pain, especially at an early age.
You should consult a doctor if your child exhibits the following symptoms: